
Critical Care Services
Welcome to James Cook Critical Care Services
The Critical Care department is committed to providing, high quality, safe and compassionate care. We understand that this can be a distressing and confusing time. Please ask questions, we are here to help.
Admission to Critical Care is for patients whose condition is serious and possibly life threatening. A patient may come to Critical Care because of a trauma, an illness, or after
a major operation. There is a multi-professional team that will care for your loved one. The nursing ratio will vary, some people require 1:1 care, others may be allocated one nurse between two patients. This is constantly assessed to ensure your loved one receives the most appropriate level of care.
The initial assessment and admission can take a long time. Whilst this happens, you may be asked to wait in the visitor’s area. We understand this can be frustrating and worrying and we will do our best to keep you informed. Seeing your loved one in Critical Care for the first time can be very distressing. They are likely to be connected to a number of machines and drips and will often look very different from how they normally look.
The patient’s condition can change a lot during their stay, sometimes improving but can also become worse. Recovery is not always possible. Some people may recover quickly but others will need to stay for weeks or even months. For certain conditions, there may be a requirement to be transferred to another hospital for more specialist care. Patients are only moved to a different hospital when it is absolutely necessary.
Who are the staff in Critical Care?
The Consultant Doctors are “Intensivists” who specialise in the care of the critically ill. They are the most senior doctors and are in charge of the patient’s plan of care and treatment whilst they are being cared for in Critical Care. You may see different Consultants on different days. Other specialist doctors will visit the unit to advise on particular aspects of care.
- Clinical Director: Dr David McIntosh
- Deputy Head of Nursing: Tom Bingham
- Matron: Karen Banks
- Ward Managers: ICU 2: Susan Mortimer, ICU 3: Gareth Cox, GCC: Elaine Cater
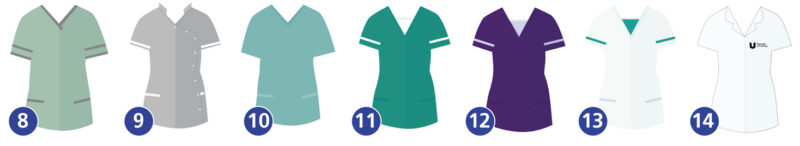
Staff uniforms

- Matron
Wearing a dark blue uniform with red trimming. The matron overseas the functioning of all the units. - Senior Staff
Wearing navy blue uniforms the nurses lead and co-ordinate our teams. - Clinical Educator
Wearing navy blue uniforms they will be working with staff to develop knowledge and skills. - Medical Team
Consultant Intensivists in dark blue scrubs. They may have their name on their top. Junior Doctors may wear other scrubs. - Nursing Staff
The nursing staff wear a light blue uniform. We have a large number of nurses. - Physiotherapists (physios)
Physios wear a white tunic with a dark blue piping. They have a wide knowledge and skill base utilised to prevent the deterioration of respiratory and muscle function. - Health Care Assistants (HCA)
HCA’s work alongside the nurses caring for your loved one and wear red uniforms.
- Domestic Staff
Wearing green tunics, they are responsible for keeping everywhere clean and tidy. - Clerical Staff
The Ward Clerks have light grey uniforms. - Advanced Critical Care Practitioner
Wearing green they have advanced skills and knowledge. - Pharmacist
Wearing a dark green, they work within the team to ensure medicines management is optimal. - Dietician
Dieticians are in purple and specialise in Critical Care ensure all our patients are reviewed and nutrition care plans optimised. - Occupational Therapist
Wearing white with dark green stripes, they help optimise recovery and comfort. - Student Nurse
A trainee nurse in a white tunic with their university symbol.
Visiting Critical Care
The current visiting times within Critical care are 12:00 until 18:00. The mornings can be very busy with doctors’ ward rounds and patients’ personal care being undertaken. Your visits may be interrupted by necessary treatments or examinations, and you may be asked to wait in the visitor’s area.
Phone numbers
- ICU 2: 01642 282680
- ICU3: 01642 854539
- General Critical Care: 01642 854898 or 01642 854523
- Email: [email protected]
This email address is monitored 08:00 until 17:00 Monday to Friday (not including bank holidays).
Please feel free to phone us at any time. However, it would be helpful to nominate one or two members of the family for telephone calls who can then relay the information given to the rest of the family. The information we can give over the telephone will be limited.
Visiting Critical Care after 22:00
After 22:00 the South Entrance will be locked. Please come to us via the North Entrance or the Maternity Entrance. We are more than happy to meet you. We will talk to you about this over the phone at the time.
Car parking
All parking on site is charged. We can provide a form to complete to apply for a parking permit free of charge for one month. Please speak to the nurse in charge for more information.
How to find us
For ICU please follow the yellow route on floor 1. For general critical care please follow the orange route on the first floor.
Hospital map
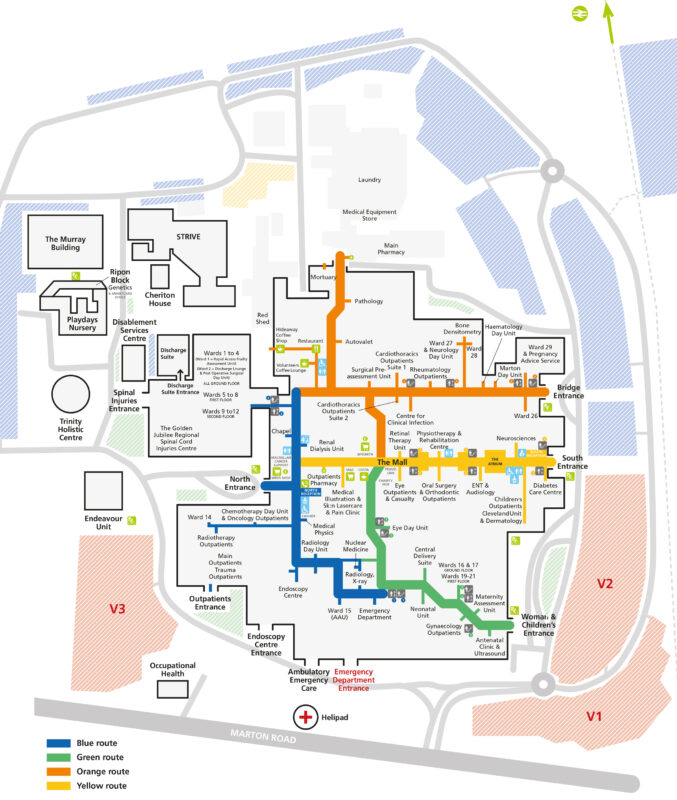
Intensive Care Unit – James Cook University Hospital
ICU equipment monitors a patient’s health and supports bodily functions until they recover.
- Bedside monitor
Displays heart rate, blood pressure, intracranial pressure, arterial oxygen saturation and carbon arterial oxygen saturation and carbon dioxide elimination. - Syringe pumps
For medicines such as insulin, adrenaline, antibiotics and pain relievers. - Infusion pumps
Delivers fluids and some medicines into the vein. - Central venous catheter
A vascular access line used to administer drugs. - Ventilator
Supplies oxygen and helps the patient to breathe. - Feeding pump
Delivering liquid food into the stomach through a tube in the nose. - External ventricular drain (EVD)
Regulates pressure around the brain draining fluid. - Humidification device
Use to deliver oxygen usually by cannula inserted into the nose. - Haemofiltration machine
Can help the kidneys in removing toxins and waste products from the blood. - Sounds
You may hear alarms and bleeps from the equipment. These help staff to monitor their patients. - Arterial line
A vascular access line used to measure blood pressure and take blood and analysis. - Warm air heating
Delivered through a special air filled blanket. - Air filled mattress
To help prevent pressure sores. - Patient diary
Used by staff and relatives to record and document an individual patient’s journey. - Patient record
Recording important data for example, blood pressure, heart rate, conscious level, intracranial pressure, urine output.
Support
You are free to touch, comfort and talk to your loved one. It may help them to hear and recognise familiar voices, even if they don’t appear to respond.
Patients’ property
We have minimal storage on the units for patients’ property, this is to allow space for the specialist equipment required to look after patients.
In the early stages of admission people will only need essentials such as glasses, teeth and hearing aids. You are welcome to bring any family photos that your relative or friend would like to display within their bed space. We have televisions and radios for patient use if they are well enough. Please discuss with your nurse if there is anything else you would like to bring in.
If your relative is admitted to us with property, we will document their belongings and ask you to take home any valuables. If valuables are unable to be returned home, they will be sent to our cashier’s office where they will be stored in a safe.
Please be aware to collect or claim these items you will be required to show proof of ID.
Patient diary
The Nursing staff will keep a diary. Each day they will write a short note of the day’s events. We will take a picture during your loved ones stay. This will be kept in a confidential file until they regain capacity and express whether they wish to keep the photo or for it to be deleted. You too can also write in the diary if you would like.
Mobile phones and photographs
Please do not use your mobile phone on the unit, visitors may use mobile devices off the unit. We do not allow photographs to be taken of patients on the units. It breaches their right to privacy and confidentiality if their consent is not given. This also includes video phone calls.
Waiting for patients to recover
This will be a very difficult time and full of uncertainty and fear. We will do our best to help with this and will always be honest and open about what is happening. However, this can be an uncertain journey. A very ill patient may improve or deteriorate very quickly and sadly, sometimes die. Critically ill patients are often very weak and it is possible for serious complications such as infection or organ failure to develop in addition to their original problem.
Can I touch and talk to my loved one?
Yes, you can. The nurses and doctors will guide you, but it is important that you speak to your loved one. This will help to orientate them and make them feel safe. Even if they are receiving drugs to keep them unconscious or calm, it is very likely that they can still hear you. You can, if you wish, kiss them or hold their hand.
Please ask the nurses if you would like to be more involved with certain aspects of your loved one’s care. We would be happy to support you with this. It is normal to feel upset and frightened at times. Please talk to us, we are here to help and are always happy to answer questions.
Psychological support
People who have been critically ill can often experience delirium. This means they develop a sudden onset of confusion. They may experience hallucinations; this can be quite scary for them. They may have difficulty remembering things and can feel quite paranoid or appear very withdrawn. They may at times become very restless and resist treatment.
Some people therefore need medication or other measures to help maintain their safety and continue their treatment.
Delirium is temporary and will resolve. However, it can last from a few hours, to several weeks or months. This can be very distressing for family and friends, but you can help by reassuring them and talking with them. Please visit the ICUSteps website for more information.
Other support and facilities
Chaplaincy
We can arrange for a priest or Chaplain of any faith to come to Intensive Care. There is a chapel on site. The hospital has a bereavement service, and we can access various other support services if required. Please visit the South Tees website for more information.
Family accommodation
We have one small overnight stay room if a family needs to stay on site. We can also give details of local hotels and residences if required. There are toilets just by the entrance of ICU and at the top of the main corridor by the lifts. Entry to any ward is via the intercom system.
Please let us know if you or other family members have any disabilities that may make this difficult to use.
There are a number of vending machines throughout the hospital. Staff will be happy to direct you or help with any other information on facilities that you may require. Please visit the South Tees website for more information.
Critical care garden
We have a dedicated critical care garden which can be visited by staff, patients and family members. As it is badge access only, you will need to be with a member of staff. Please ask a member of staff for more details.
Food and drink
The James Cook University Hospital Voluntary Services Coffee Lounge
- Located on bridge entrance corridor (orange route)
- Profits donated to hospital
- Open Monday to Friday 9.30am to 6pm.
Lavazza Coffee Shop
- Located at the far end of the staff restaurant
Open Monday to Friday, 8am to 2pm.
Costa Coffee
- Located on the mall (yellow route)
Open 7am to 10pm daily
M&S Simply Food
- Located on the mall (yellow route)
Open Monday to Friday, 7am to 9pm and weekends 8am until 8pm.
WHSmith
- Located on the mall (yellow route)
Open Monday to Friday, 7am to 9pm.
Shop @ WRVS
- North entrance
Open Monday to Friday, 9.30am to 5pm and Saturday, 9am to 6pm. - Women and children’s entrance
Open Monday to Friday, 9.30am to 4pm and Saturday, 9.30am to 3pm.
Cash points
- North entrance reception, near WRVS and Macmillan Support
- WHSmiths located in the mall
- You can also get cash back when purchasing something in M&S.
Looking after yourself
You can help the patient by taking care of yourself. You shouldn’t feel guilty for not being by their bedside 24 hours a day. You need to give yourself a break and this will also give your relative or friend time to rest. The Intensive Care staff will care for your loved one throughout the day and night. They will contact you straight away if they need to or if there is any significant change in their condition.
Your family and friends will be concerned about you and the patient, and they will want to know how things are. You may appreciate their concern, but it can be tiring if the phone is ringing all the time when you’re at home between visits to the hospital. Passing on the information by e-mail or text message to several people at once can be easier, or, you could speak to one person regularly and they could pass the information on to others on your behalf.
You may not feel like eating and you may have difficulty sleeping but do take time to eat regularly and rest when you can. If you become tired and ill, you won’t be able to care very well for the patient. For more information please visit the ICUSteps website.
If the patient is your partner
If the patient is your partner, you may suddenly feel very alone. Accept offers of help from friends and family. You will have less time to do things like shopping and may need help with childcare.
Often, in times of worry and stress, people turn to their partner for support. If you don’t feel like you can tell other family members about your worries of what may happen in case you upset them, you could get help from one of the organisations; Mind, Samaritans, Trauma Headway. Please ask for more information from the nurse in charge.
Make sure that your bills are being paid and if you need to get access to your partner’s bank account, contact your bank and explain the situation. You may be able to get temporary control of the account while your partner is not able to deal with these things.
If financial constraints are a worry, contact the Citizens Advice Bureau for help and advice.
Day One – Trauma Support
Day one is a national charity supporting lives affected by major trauma. They provide practical and emotional support, alongside NHS clinical care, for patients and their loved ones. For more information, please visit the Day One Trauma Support website.
Leaving critical care
Once considered well enough, patients will be stepped down and be transferred to a ward. The more normal atmosphere of a ward is an important step in the right direction and patients are only moved when the team feel they are ready. However, it is important to understand that the patient’s journey to recovery continues on the ward and they may still require further input from Intensive Care. You may feel anxious about the move. If so, please speak to us.
ICU Steps
ICU Steps Tees is a support group for previous ICU patients, their families and friends run by former intensive care patients, relatives and health professionals. It was developed to provide on-going support after discharge for patients and relatives who have been affected by critical illness.
For more information and dates of upcoming support groups, please visit the ICUsteps website.
End of life
Our aim is to help everyone to return to good health, sadly despite our best efforts this is not always possible. Our team will work with specialist teams to discuss the next steps and your loved ones wishes, this may include talks about organ donation. For more information, please visit the ICUsteps website and the Organ Donation website.
Feedback
Your feedback is really important to us. Please talk to the nurse in charge about how you can leave feedback or visit the critical care survey website.
Call for Concern C4C
Call for concern is a patient safety service for adult patients, families, and friends to call for help and advice if you or your family are concerned that there is noticeable change or deterioration in condition whilst within a ward area.
For more information, please visit the South Tees website.
Complaints
The staff do all they can to keep relatives informed about what treatment is given and why. Where possible, they will let the patient and relatives know what treatment options they have. If there is anything you don’t understand or want to know more about, please speak to the staff on the unit.
If you’re unhappy with the care being given, please speak to our team about this.
If you feel you are not able to resolve concerns in this way, you can contact the hospital Patient Advice and Liaison Service (PALS) who will help you to find the answers you need.
For more information, please visit the South Tees website.
Useful contacts
Other organisations may be able to offer further information and support.
Please visit the ICUsteps website.
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]