

Clinical Diagnostic and Support Services
This booklet is designed to give some information about how the children’s physiotherapy team at The James Cook University Hospital will help you in your recovery following your operation.
- Chest care
- General mobility
- Postural advice
The exercise instructions in this booklet are given as a general guideline only as each patient is treated as an individual.
Physiotherapy before your operation
A physiotherapist may see you prior to your operation in your pre-assessment clinic appointment or on the ward at the time of your admission.
What to expect after your operation
Following your operation you may require oxygen support whilst recovering within paediatric critical care unit.
You will be attached to monitors, a catheter, drains from your wound site and lines for your drugs or fluids. This is all routine and nothing to be concerned about.
You will start to sit of out bed on the first day after your surgery and each day you will gradually increase how much you walk on the ward assisted by the physiotherapy and nursing staff.
Your mobility should improve each day, and you will soon be able to walk on your own again.
Walking soon after your surgery is encouraged as it will improve your lung function. Lack of walking at this stage and spending too much time in bed could lead to a chest infection. It will be normal to experience discomfort on exercise, but it will improve with time as you do more.
Chest care
Deep breathing exercises begin immediately after your operation. Some people become chesty in the first few days following surgery due to extra mucus production as result of:
- Having an anaesthetic
- The discomfort or pain from your wound limiting you from taking in deep breath and coughing
- Reduced mobility in the first few days after surgery
Your physiotherapist will assess your breathing and how your lungs are working. They may advise on the ideal position to improve your comfort and lung function.
Breathing exercises are advised every few hours post-surgery and you may have been given an incentive spirometer.
Deep breathing exercises aimed to keep your lungs clear, after your operation, together with huffing and coughing.
How to do your deep breathing exercises
These activities involve axial loading (spine being pressed down) and can cause pain or make it worse.
- Sit upright with your hands placed over the sides of your chest
- Take a deep breath in slowly through your nose
- Hold this breath in for one to two seconds and then breathe the air out slowly through your mouth
- After 5 breaths do a huff, repeat five times
To do a huff – take a breath in then force the air out quickly through an open mouth, as if you are steaming a window.
If you have any phlegm in your throat take a deep breath in and have a good strong cough. Afterwards, take normal relaxed breaths.
Incentive spirometry
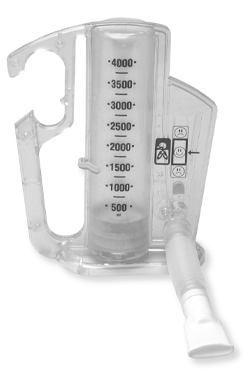
You may be given an incentive spirometer (as shown below) before your surgery to use. We will continue to use it after your surgery so please bring it with you into hospital. It is best to use whilst sitting upright.
To use your incentive spirometer:
- Take a long, steady breath in through the mouthpiece, keeping the small yellow disc in the smiley face
- Aim to get the large yellow disc as high up in the cylinder as possible
- Move the yellow marker on the side to show how high it reached
General mobility
Your physiotherapist will encourage you to progress your mobility from day one after your operation.
The physiotherapist will monitor and assess your ability to do simple tasks during your hospital stay. Any problems will be identified and treated as appropriate in conjunction with other members of the team.
Most patients are usually discharged home between 4 to 7 days after their operation, although this depends on their recovery.
Exercises
From the first day after your surgery we will encourage you to begin exercising. This may initially involve some gentle arm and leg exercises to prevent stiffness, help circulation and increase general mobility. Repeat each exercise two to three times per day.
Arm exercises
- While standing or seated, raise both arms up above your head as pain allows, then back down
- Repeat five to ten times
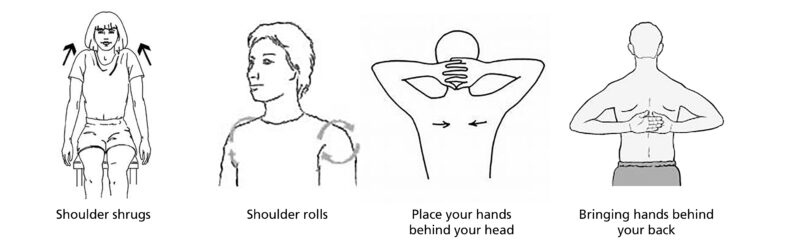
- Gentle shoulder shrugs (up and down) and shoulder rolls (forwards and backwards)
- Place your hands behind your head. Bring your hands behind your back. Slowly stretch your hands up towards your shoulder blades
Circulatory exercises:
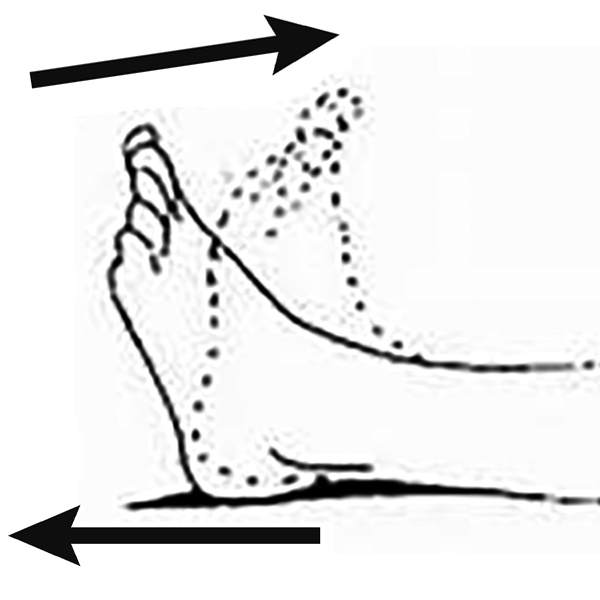
- Bend and straighten your ankles and toes
- Repeat ten times on each foot
- Circle your feet from your ankles round in one direction and then repeat in the other direction
- Repeat ten times each direction and on each foot
Leg exercises:
- Tighten your thigh muscles on the front of your legs by pressing the back of your knee into the bed and pulling your toes towards you
- Squeeze your thigh muscle and hold for 5 seconds
- Repeat 5 to 10 times on each leg
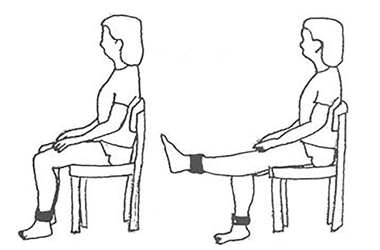
- Straighten one leg out in front of you whilst sitting
- Hold for five seconds, and then relax
- Repeat 5 to 10 times with each leg
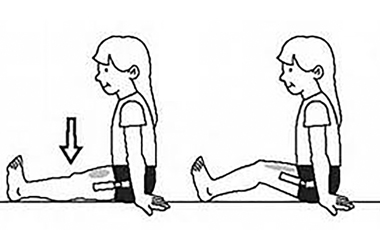
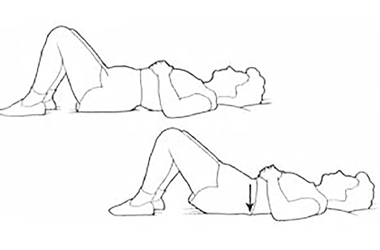
Pelvic tilting:
- Lay on your back with your knees bent so your feet are flat on the bed
- Gently arch the bottom of your back, hold for 3 seconds then flatten your back by pressing your lower spine on the bed
- Try and increase the amount of movement you can achieve each time
- Repeat 5 to 10 times
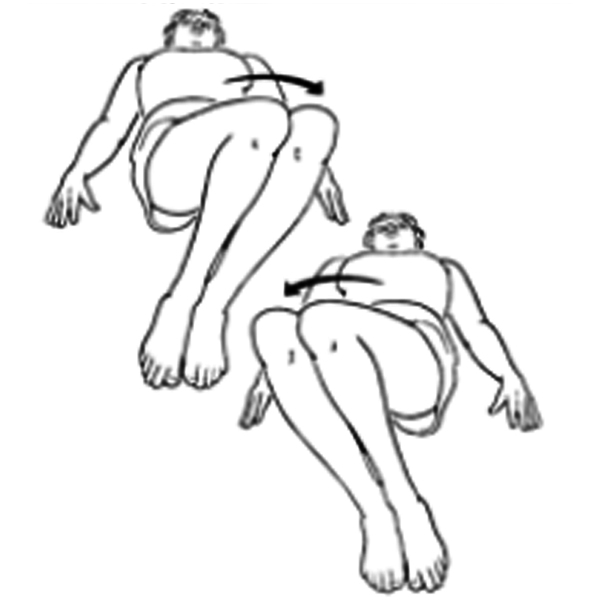
Knee rolls:
- Lay on your back with your knees bent and your feet flat on the bed
- Keeping your knees together slowly let your knees fall out to the right side
- Only move them within a comfortable range
- Stop and bring them back to the middle
- Then repeat letting your knees fall to the left side
- Repeat 5 to 10 times to each side
Knees to chest:
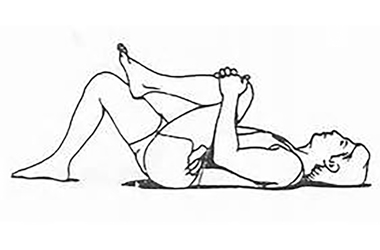
- Lay on your back with your knees bent and feet flat on the bed
- Bring one knee towards your chest at a time
- Hold for 5 seconds and then relax
- Repeat 5 to 10 times
- Then change legs and repeat
Postural advice:
At first you may feel like you are leaning to one side when sitting or standing. This is a normal feeling and it can take time to adjust to your new posture. The muscles that support your spine will take time to adapt after your surgery.
Top tips:
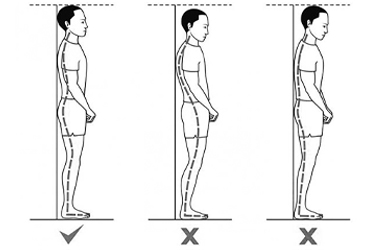
Try standing in front of a mirror to help in adjusting and seeing what your new posture looks like. It is easier to correct when you can see what you look like
Ask your family and friends to remind you to stand or sit up tall when you are with them.
Try standing with your back to a wall pushing your shoulders back so they touch the wall.
After discharge from hospital
After your operation, your lung function should improve and your ability to exercise will also gradually increase.
Exercise after discharge
- Improves your fitness after your operation and should become part of your daily routine.
- Should start immediately after discharge from hospital.
- Walking distance should be increased gradually.
Contact details
- Ward 22:
Telephone: 01642 854522 (24 hours) - PCCU:
Telephone: 01642 854667 (24 hours) - Mr Zak Choudhury’s secretary
Telephone: 01642 835564 - Mr Prasad Karpe’s secretary
Telephone: 01642 835811 - Ms Toni Isaacson’s secretary
Telephone: 01642 850850 extension 55310 - Cheryl Honeyman, Nurse Specialist
Office Telephone: 01642 850850 extension 56266
Mobile number: 0793 536 1881
Email: [email protected] - General enquiries
Email: [email protected]
Useful websites:
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, i.e. braille or large print.
T: 01642 835964
E: [email protected]
The James Cook University Hospital, Marton Road, Middlesbrough, TS4 3BW.
Telephone: 01642 850850
