
Maternity
Having more than one baby
Finding out you are having twins, triplets or even quadruplets can be exciting, but it can also be an anxious time for you, your partner and family members. If you are expecting more than one baby, it is important that you are well prepared for the changes that will take place during your pregnancy and after the babies’ birth.
A ‘multiple pregnancy’ is the term used when you are expecting two or more babies at the same time. It occurs in about one in 80 pregnancies. Fertility treatment increases the chances of multiple pregnancy.
The information in this booklet provides an overview of multiple pregnancy and care offered by South Tees Hospitals NHS Foundation Trust.
Further information and support is available from your midwife and obstetrician and from the multiple pregnancy organisations listed at the end of the booklet.
Congratulations on your new babies!
An exciting adventure begins…

On this page
Types of multiple pregnancy
At your early ultrasound scan which confirms whether you are carrying twins or triplets, it is also important to determine “chorionicity” of your pregnancy. This helps to identify if your babies share a placenta (the afterbirth).
This is important to know, as babies who share a placenta (monochorionic) have a higher risk of complications.
If your babies share a placenta, they are identical or ‘MONOZYGOTIC’.
Most babies who do not share a placenta are non-identical or ‘DIZYGOTIC’.
However, it is also possible for babies not sharing a placenta (dichorionic) to be identical as well, as nearly a third of monozygotic (identical) twins will each have their own placenta. Therefore, these will have the same appearance on ultrasound scans as the DCDA (non-identical or dizygotic) twins.
Dichorionic – two placentas
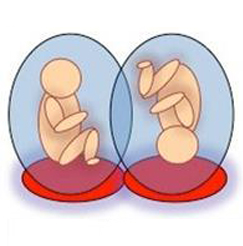
Monochorionic – one placenta
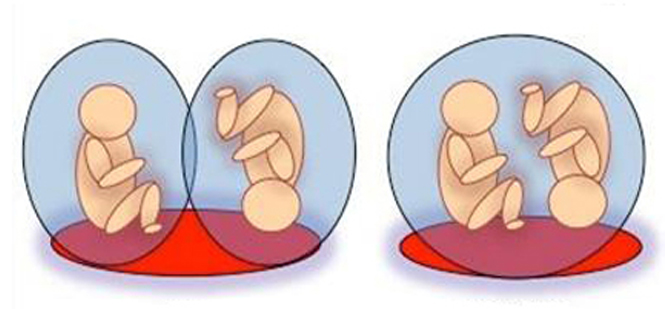
Twins

Dichorionic Diamniotic (DCDA)
Each baby has its own placenta with its outer membrane called a ‘chorion’ and its own amniotic sac. This happens if two eggs are fertilised at the same time or if one egg splits into two soon after fertilisation. Two thirds of DCDA twins are non identical.
Monochorionic Diamniotic (MCDA)
The babies share a placenta and chorion but they each have their own amniotic sac. This happens if a single fertilised egg splits a little later. These babies are always identical.
Monochorionic Monoamniotic (MCMA)
Rarely, the fertilised egg splits later still. In this case, the babies will share a placenta and chorion and are within the same amniotic sac. These babies are always identical. This type of twins carries additional risks.
Triplets
Triplets can be:
- Trichorionic: each baby has a separate placenta and chorion
- Dichorionic: two of the three babies share a placenta and chorion and the third baby is separate
- Monochorionic: all three babies share the same placenta and chorion
Significance of multiple pregnancy
Most women who have a multiple pregnancy have healthy pregnancies and healthy babies. However, complications are more common in multiple pregnancy and having extra care during your pregnancy including more ultrasound scans reduces these risks to you and your babies.
Your health
1. Pregnancy symptoms
Because you are carrying more than one baby, your body has to work extra hard! Symptoms of pregnancy (experienced by many pregnant women) are therefore more common in a multiple pregnancy. These include:
Heartburn
Swollen ankles
A bigger bump than if you were having just one baby
Varicose veins
Backache
Tiredness
Fortunately, these symptoms don’t last forever!
They get better naturally after the babies are born.
2. Pregnancy complications
Any complications of pregnancy are more common with twins.
This includes:
- Anaemia – this is usually caused by a shortage of iron because developing babies use up a lot of iron
- Pre-eclampsia – a condition that causes high blood pressure and protein in your urine; further information on pre-eclampsia can be found by visiting the RCOG website
- A higher chance of bleeding more heavily than normal after the birth – doctors and midwives are trained to deal with these situations
- A higher chance of needing a caesarean section or assisted vaginal delivery to deliver your babies. (See ‘Planning for Delivery’ Section.)
Your babies’ health
1. Prematurity
You are more likely to have your babies early if you are expecting twins or triplets.
- About 60 in 100 sets of twins will be born spontaneously before 37 weeks of pregnancy
- About 75 in 100 sets of triplets will be born spontaneously before 35 weeks
In comparison, only about 10 in 100 women who are pregnant with one baby will give birth before 37 weeks.
Babies born under 34 weeks of pregnancy will need to be cared for on the neonatal unit. Having a baby born early can be worrying and distressing for parents. You will be supported to spend as much time as possible with them.
Babies born after 34 weeks may be able to be cared for on the Transitional care ward. When on the Transitional care ward you will be able to stay with your babies as the main care giver, supported by the midwifery and neonatal team.
Your babies may require a longer stay in hospital to support their transition to life outside the womb including temperate control and feeding.
2. Problems with growth
Having more than one baby increases the chance of the placenta not working as well as it should. This can affect the babies’ growth and wellbeing.
3. Twin-to-twin transfusion syndrome (TTTS)
Twins sharing a placenta (monochorionic pregnancies) also share the blood supply. In around 15 in 100 monochorionic twin pregnancies, the blood flow may be unbalanced. We call this twin-to-twin transfusion syndrome (TTTS).
One baby, the ‘donor’, receives too little blood and has a low blood pressure while the other baby, the ‘recipient’, receives too much blood and has a high blood pressure. You will be monitored with frequent scans for signs of TTTS.
It can be mild and may not require any treatment, or it can be serious, in which case you will be offered treatment in a hospital (St George’s Hospital in London), with specialist expertise for further care. This involves using a laser to separate the two circulations.
Important
If you experience any sudden onset of abdominal swelling and, or discomfort please contact the Maternity Assessment Unit (MAU) to have an urgent assessment and scan.
Care during pregnancy
You will be under the care of a specialist healthcare team, which will usually include an obstetrician and a midwife who specialises in multiple pregnancies.
- All monochorionic twins and most dichorionic twins will be seen in a consultant led specialist twin clinic in The James Cook University Hospital (JCUH).
- Some dichorionic twins may be seen in Friarage Hospital or a different antenatal clinic in JCUH.
Screening
Like all women, you will be offered a scan at about 12 to 14 weeks to screen for chromosomal conditions such as Down’s syndrome. These scan results can be combined with results from a blood test to assess the risk of one or both of your babies having a chromosome problem.
You will also be offered another scan at around 20 weeks to look at your babies’ development. The chance of these tests finding a problem is slightly higher than if you were pregnant with only one baby.
Growth scans
Having a multiple pregnancy means that you will need more visits to the antenatal clinic at your hospital. You will be offered extra ultrasound scans to monitor your babies’ growth more closely.
- Dichorionic twins
Scans about every 4 weeks from 20 weeks of pregnancy onwards - Monochorionic twins
Scans every 2 weeks from 16 weeks of pregnancy onwards
Medication
You may be advised to take iron tablets and folic acid each day throughout your pregnancy.
If you are having twins and have any other risk factors for pre-eclampsia, you may be advised to take low-dose aspirin from 12 weeks of pregnancy onwards to reduce the risk.
Advice and information
During your pregnancy your doctors and midwives will give you information and advice about:
Planning the birth, including timing and types of birth and pain relief
Looking after your babies following birth
Care for you after your babies are born, including contraception
Planning for delivery
Timing
You may go into labour early with multiple pregnancy. Even if you don’t, you will be advised to have your babies before your due date (elective birth). This is done either by having labour started off (induced) or by having a caesarean section.
The exact timing of delivery for multiple pregnancy depends on individual circumstances. If your pregnancy has been uncomplicated, it is generally advised that you should be offered elective birth from:
- 37 weeks
If you are carrying dichorionic twins (babies having separate placentas) - 36 weeks
If you are carrying monochorionic twins (babies sharing a placenta) - 35 weeks
If you are carrying triplets
If you have any concerns about having your babies born at these recommended times, you should talk to your healthcare professional, as continuing the pregnancy beyond these dates increases the risk of harm to your babies.
Location
You will be advised to give birth in the consultant-led maternity unit in The James Cook University Hospital, Middlesbrough, which has a neonatal unit. You can also get help from doctors if needed.
Type of delivery
You will be able to discuss your birth plan with your midwife and obstetrician. Your decision whether to have a vaginal birth or a caesarean section will depend on several factors including presentation of the presenting twin, position of the placenta(s), how the babies are growing and whether you have had a previous caesarean section.
Both vaginal birth and caesarean section have benefits and risks, and it is important to consider the options carefully and to talk about your individual situation with your healthcare professionals.
Your own preference is important and you should be given enough time to consider all of the relevant information before deciding what suits you best.
Triplets, quadruplets and monoamniotic twins
These babies are usually delivered by caesarean section unless you are in very premature labour or you give birth to the first baby very quickly.
Diamniotic twins
If the baby nearest to the neck of the womb (often called the presenting twin) is head-down and you have no other complications then you should be able to have a vaginal birth if you wish. The position of your second twin can change after the first baby is born and should not influence how you choose to give birth.
Labour and birth
Unexpected labour
If you have decided to have a caesarean section but go into labour naturally, you should go straight to hospital. If appropriate, the operation will be done as soon as possible. However, occasionally labour may be too advanced and it may be safer for you and your babies if they are born vaginally.
If you go into labour very early in the pregnancy, you may be advised that it would be better for your twins to be born vaginally.
Monitoring your babies during labour
Monitoring your babies’ heartbeats during labour is recommended; it shows us how well your babies are coping and helps us make decisions to enable safe delivery. Unfortunately, this monitoring may make it less easy for you to move around.
We are sometimes unable to monitor both babies using the bands strapped around your tummy. If this is the case, your first baby’s heartbeat may be monitored by applying a clip onto your baby’s head via your vagina.
Pain relief during labour
You may wish to have an epidural for pain relief. This can be helpful if any complications arise and your babies need to be delivered by caesarean section, forceps or suction cup (vacuum or ventouse). However, it is not essential and alternative pain relief should be discussed with you.
After the first baby is born
After your first baby is born, the cord will be clamped and cut in the usual way but the placenta will stay inside the womb until your second baby has been born. If possible this is a good time for your partner to do skin to skin with your baby. Your midwives will explain why skin to skin with baby is so important.
Your midwives and doctors will check whether your second baby is coming head-first or bottom-first by feeling your tummy, doing an internal examination and by carrying out an ultrasound scan.
As your second baby comes down the birth canal, the second bag of waters may be broken. A normal birth usually follows within about 30 minutes to an hour.
Although it is uncommon for the first twin to be born vaginally and the second to be born by caesarean section, it can occur if the second baby needs to be delivered urgently and, or a vaginal birth would be unsafe.
This can happen anywhere between two and ten in 100 vaginal twin births. Skin to skin can also be carried out by you or your partner if your baby is born by cesarean section.
Staff present at delivery
The delivery room may seem crowded when your babies are being born. People who may be in the room include:
- At least one midwife (often two)
- An obstetrician (in the delivery room or close at hand)
- Doctors and nurses specialising in the care of newborn babies
- An anaesthetist, to help with pain control.
Looking after your babies
Looking after multiple newborns can be a very busy time for you and your household. It is quite natural to have concerns about how you are going to manage looking after more than one baby.
Feel free to talk to our staff about any questions or concerns that you have. Your specialist multiple pregnancy midwife is often a great source of information and reassurance.
Tips:
Be willing to accept help when it is offered
Establish a routine as early as possible
Look out for activities and support groups in your local area
Pregnancy, birth and beyond
As well as your routine antenatal and postnatal care, the community Midwifery and Health Visiting service run Parent Education sessions designed especially for multiple pregnancy.
We highly recommend these sessions, as they provide helpful advice, support and information. Ask your specialist midwife about these sessions.
Feeding
Midwives will give you lots of information during your pregnancy to help you make an informed decision around how to feed your babies. Even though you’re having more than one baby, your body is capable of producing enough milk to breastfeed your babies.
Don’t let the fact you are having twins (or triplets) put you off breastfeeding. If you encounter difficulties, your midwives can offer you advice and support.

Key points
Multiple pregnancy occurs in about one in 80 pregnancies
While most women with multiple pregnancies will have a healthy pregnancy and healthy babies, complications are more common
Extra antenatal checks and ultrasound scans to monitor your babies will be offered
You are more likely to have your babies early if you have a multiple pregnancy
You will be advised to give birth in a consultant-led maternity unit
Your midwives and local support groups can provide you with advice and support after your babies are born
Further information
Further information can be found by visiting the following websites
Multiple pregnancy
- Twins trust
- National Institute for Health and Care Excellence (NICE)
Multiple pregnancy: Antenatal care for twin and triplet pregnancies
Screening
Premature labour
National Institute for Health and Care Excellence (NICE):
Preterm Labour and Birth
Heavy bleeding after birth
RCOG patient information:
Heavy bleeding after birth (postpartum haemorrhage)

Sources and acknowledgements
This leaflet has been developed by the team in The James Cook University Hospital, led by:
- Dr Vedrana Caric, Consultant.
- Dr Yong Sheng Tan, Foundation Doctor
- Lynn Whitecross, Multiple Birth Midwife
- Dr Saroj Dalmia, Specialty Registrar in Obstetrics and Gynaecology
- Rebekah Young, Medical Student
We are very grateful to the parents of beautiful twins and triplets who agreed for us to use their photos.
This leaflet is based on the RCOG patient leaflet: Multiple pregnancy: having more than one baby, NICE clinical guideline Multiple pregnancy: Antenatal care for twin and triplet pregnancies, and the RCOG Green-top guideline management of monochorionic twin pregnancy, which you can find on the RCOG website.
The guidelines contain full lists of the sources of evidence used.
This leaflet was reviewed before publication by women attending our multiple birth clinics in The James Cook University Hospital and women who were looked after and delivered twins or triplets in our hospital.
Contact
- The James Cook University Hospital Maternity Department
Advice line: 01609 763093 - Non urgent communication regarding twins
Email: [email protected]
Please add your name in the subject title.

Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]