| Name: |
| Hospital Number: |

Cardiac Rehabilitation
Exercise or physical activity and your heart
Your heart is a muscle which pumps blood around your body. Exercise can help your heart muscle to become fitter so that it can pump blood more efficiently around your body.
The type of exercise that improves your hearts fitness the most is called aerobic exercise.
Examples of aerobic exercise are:
Walking
Cycling
Swimming
Dancing
NICE (2007) recommend that we should aim to be physically active or exercise for 20-30 minutes daily to the point of breathlessness. The aim of this programme is to help you work towards this.
The British Heart Foundation recommend that exercise or activity is performed at a moderate intensity. Exercising at a moderate intensity means that you should be working hard enough to be breathing more heavily and feeling warmer but not so hard that you are unable to talk and exercise at the same time.
More information can found by visiting the NICE website and the BHF website
The cardiac rehabilitation sessions
We run an eight week course of cardiac rehabilitation. Each session lasts for two hours. The exercise component of the session is approximately 45 minutes followed by a relaxation session and a health education topic.
We will also help you to plan what activity or exercise is appropriate for you to do in between each of your sessions.
Your cardiac rehabilitation course will commence on:
| Venue: |
| Date: |
| Time: |
| Tutor: |
The James Cook University Hospital
Cardiac Rehabilitation Gym
1st Floor (next to ward 30)
(Use bridge entrance)
The James Cook
University Hospital
Middlesbrough
TS4 3BW
The Friarage Hospital
Northallerton
North Yorkshire
DL6 1JG
The Friary Hospital
Multi purpose room
Queens Road
Richmond
North Yorkshire
DL10 4A
Redcar Primary Care Hospital
Crossley Unit (1st Floor)
West Dyke Road
Redcar
TS10 4NW
The Neptune Centre
Community Room (1st Floor)
Ormesby Road
TS3 7RP
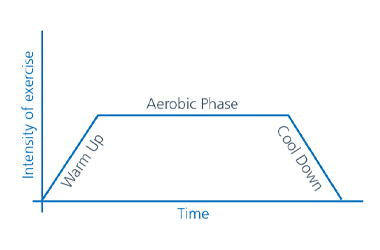
Each exercise session will include:
- Warm up
To ensure your body, particularly your heart and muscles are ready for the aerobic exercise. This lasts approximately 15 minutes and comprises general mobility, pulse raising exercises and simple stretches. - Aerobic circuit
This lasts approximately 20 minutes and comprises a circuit of aerobic exercise. The aim of this is to raise your heart rate to your individual goal. This will have been set up for you at your initial assessment appointment. - Cool down
This lasts approximately 10 minutes and comprises walking, gentle mobility and simple stretches. This is important to allow your heart rate to gradually return to your resting level.
Exercise is done at your own pace and should be enjoyable.
We will take your pulse and blood pressure in the class at every session and you will use a ‘how it feels’ scale known as the BORG scale to make sure you are exercising at the right level.
Borg scale instructions
While exercising we want you to rate your perception of exertion, for example, how heavy and strenuous the exercise feels to you.
The perception of exertion depends mainly on the strain and fatigue in your muscles and on your feeling of breathlessness or aches in the chest.
Look at this rating scale; we want you to use this scale from 6 to 20, where 6 means ‘no exertion at all’ and 20 means ‘maximal exertion’.
Try to appraise your feeling of exertion as honestly as possible, without thinking about what the actual physical load is. Don’t underestimate it, but don’t overestimate it either. It’s your own feeling of effort and exertion that’s important, not how it compares to other people’s. What other people think is not important either. Look at the scale and the expressions and then give a number.
The Borg Scale:
| 6 | No exertion at all |
| 7 | Extremely light |
| 8 | |
| 9 | Very light |
| 10 | |
| 11 | Light |
| 12 | |
| 13 | Somewhat hard |
| 14 | |
| 15 | Hard (heavy) |
| 16 | |
| 17 | Very hard |
| 18 | |
| 19 | Extremely hard |
| 20 | Maximal exertion |
9 corresponds to ‘very light’ exercise
For a normal healthy person it is like walking slowly at his or her own pace for some minutes.
13 on the scale is ‘somewhat hard’ exercise
But it still feels OK to continue.
17 ‘very hard’ is very strenuous
A healthy person can still go on, but he or she really has to push him or herself. It feels very heavy and the person is very tired.
19 on the scale is an extremely strenuous exercise level
For most people this is the most strenuous exercise they have ever experienced.
Important
At each session it is important for us to ensure that you are fit to exercise and we would ask that you let us know if you have experienced any of the following in between each session:
Illness or fever including coughs, colds and tummy upsets
Increased breathlessness
Angina symptoms coming and going at rest
Palpitations or an irregular heart beat
Dizzy spells
Persistent back pain or chest pain
Swollen ankles or feet
Problems with your diabetes
Joint and muscle problems likely to limit your exercise tolerance
Any changes to your medication regime
Any other issues you feel are important
Occasionally after discussing some of these issues with you we may advise that it is not appropriate for you to exercise on that day.
If you experience any of these symptoms during your usual daily exercise and activity other than in the sessions you can ring the cardiac rehabilitation department or your GP or NHS direct for further advice.
General information
We look forward to you joining us. We hope that you enjoy your cardiac rehabilitation course. To ensure that you and the rest of the group get the most out of the programme we do have some ground rules.
If you are unable to attend a session please let you tutor know either the week before or by telephone on 01642 854644.
If you do not attend for 2 weeks running and you have not let us know you will automatically be discharged from the service.
- If you need to leave early please inform the class tutor at the beginning of the session
- Unfortunately due to demand on the service if you miss sessions we are unable to add these onto the end of the programme.
Do
Do remember to take your medication before you attend the session and remember to bring any medication with you that you may need to take during the session for example; GTN or inhalers
Do follow the exercise advise that is given to you by the class tutors
Do try to respect and support others in the group and maintain confidentiality
Do turn off you mobile phone or put it on silent during the class
Do wear suitable loose fitting clothing and flat shoes (not flip flops) during the exercise. If you wear glasses or hearing aids bring them with you.
Do, if you are diabetic ensure you check your blood sugar prior to attending your class and inform the tutor of the reading.
If your blood sugar (BM) is above 15 you will not be able to participate in the exercise session.
Don’t
Don’t attend the session if you are unwell
If you have angina type chest pain follow the advice on your GTN cardDon’t bring valuables with you to the class
South Tees NHS Foundation Trust can not take responsibility of loss or damage to property
Partners are welcome to attend the sessions and join in with the health topic and discussions. Unfortunately partners cannot participate in the exercise session.
The good news about physical activity
Increasing your levels of activity can make a big difference to the quality of your life.
You can experience:
Better health
More energy
Reduced stress
You may find it easier to relax and it may also help improve your sleep
Stronger bones and muscles which can improve your balance, strength, suppleness and mobility
More independence
Easier to maintain a healthy weight
Opportunities to meet other people
Increased enjoyment of life
To get the most out of your exercise you should aim to exercise for at least 30 minutes on five occassions during the week.
Managing your own activity or exercise plan at home
- Think of exercise or activity as a normal part of your everyday life
- Choose a variety of exercises and activities that you enjoy
- Start slowly and gradually build up the length of time that you spend on your chosen exercise or activity
- Try to do something everyday
- Set yourself realistic goals
- Wear loose comfortable clothes and appropriate footwear
- Remember the warm up and cool down are important part of your exercise sessions
- Simple stretches can help you to avoid injury and we have included some in this booklet similar to the ones that are used at your cardiac rehabilitation sessions. If there are any stretches that you have been advised not to perform during the rehabilitation class, please do not include them in your own exercise programme.
Some points to remember when you are undertaking any exercise or activity
- Wait at least two hours after a meal before exercising
- Do not exercise if you feel unwell – remember if you are unsure whether you should be exercising then seek advice
- Wrap up warmly on cold days and consider alternative forms of activity if the weather is too cold or windy to go out
- If you are out walking take a mobile phone with you and tell someone when you will be back
- Remember to take your GTN spray with you (if it has been prescribed for you)
Remember that changing a few of your daily habits can soon add up to you having a more active lifestyle. Every little helps!
At each of your sessions we will discuss with you an individual exercise plan for your use at home in between each of your cardiac rehabilitation sessions.
Stretches to help you warm up and cool down
Do the stretches smoothly and hold for around 8 to 10 seconds during the warm up, and 15 seconds during the cool down.
Do not bounce or jerk. If you feel unsteady hold onto a wall or sturdy chair for support. These stretches should not be painful or hurt, but you should feel a gentle stretch along the muscles indicated.
Some stretches have an alternative way of doing them.
You only have to do one method (whichever is easiest for you).
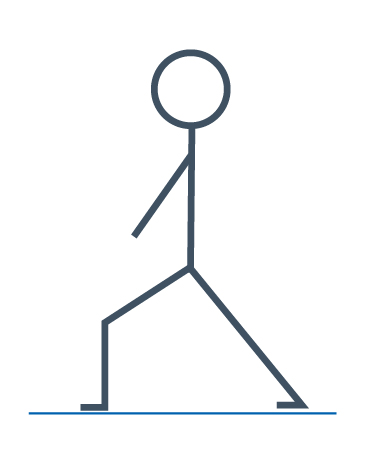
Calf stretch
Place one foot in front of the other with the front leg bent and the back leg straight. Keep the heel of the back leg on the floor, bend the front knee until you feel a stretch in you calf.
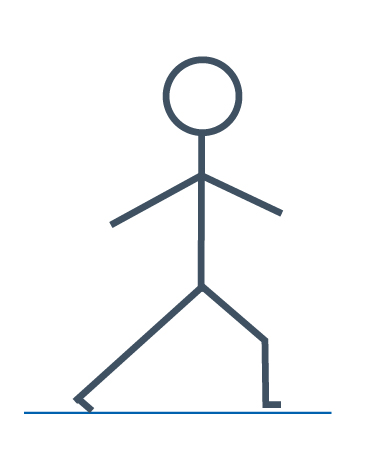
Split stretch
With your feet just over shoulder width apart and feet pointing forward, place your hands on your hips and bend one knee to take your weight over on one leg. Keep the other leg straight and both feet flat on the floor. Bend the knee until you feel a stretch in your inner thigh.
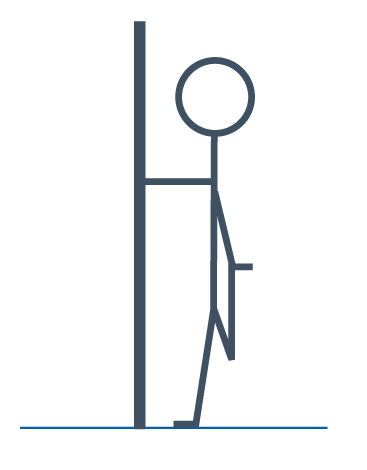
Thigh stretch
Holding onto a wall or sturdy chair or table bend the leg furthest away from the wall, hold your ankle or trouser leg and gently pull your foot towards your bottom. Try to keep your knees together and body upright. You should feel a stretch in the front of your thigh.

Or standing on one leg, stretch the other one out behind you with the tips of your toes on the floor. Gently push your hips forward until you can feel a stretch over the front of your hip and down the front of your thigh.
Hamstring stretch
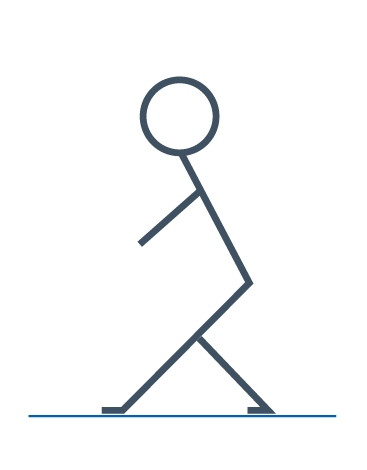
With both feet together, bend both knees. Slide one foot forward so that the front leg is straight, while the back leg remains bent. Place your hands onto the bent knee for support. You should feel a stretch in the back of your thigh, if not lift the toes of your front foot off the floor so that you are resting on the heel.
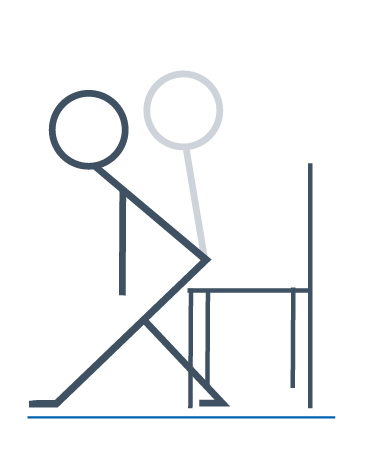
Or sitting on the edge of a chair, slide one foot forward so that the front leg is straight while the back leg remains bent with your foot flat on the floor.
Place your hands onto the bent leg for support. You should feel a stretch in the back of your thigh, if not lift your toes of your straight leg off the floor so that you are pushing on the heel.
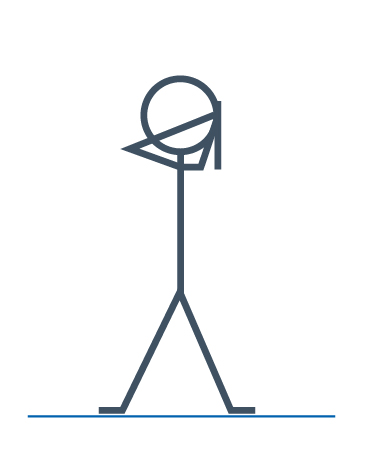
Arm stretches
Bend your arm so that your hand is on your shoulder. Slide your hand over your shoulder towards your shoulder blade. With the opposite arm gently push the arm back until you feel a stretch down the back of your arm
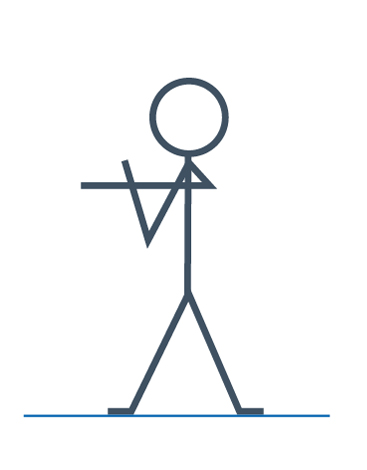
Also keeping your arm straight, take it across your body at shoulder height. Use the other arm to gently hug your arm into your body so that you feel a stretch along the back of your arm.

Chest stretch
Place your hands on the small of your back and press your chest forward until you can feel a gentle stretch across the front of your chest.
Or hold your hands together behind your back. Keeping your arms straight, lift your arms away from you until you can feel a stretch across your chest.
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]