Cardiovascular services
| Operation: |
| Operation date: |
| Date of discharge: |
Thoracic Team, Ward 32, The James Cook University Hospital
Telephone: 01642 854532
Available Monday to Friday, 7.30am until 6.00pm
Email: [email protected]
Please note: We are unable to respond to emails outside of normal office hours.
Recovering
It may take many weeks or months to recover from a lung operation. Some people recover more quickly than others. You need to pace yourself and try not to do too much, too soon.
You need to avoid:
- Heavy lifting
- Straining your arm on the affected side
- You can slowly build up your strength and fitness with light exercise, such as short walks. It is important to keep doing any exercises the physiotherapist has given you.
To help your recovery, try to:
- Eat healthly
- Get enough rest
- Do light exercise
- Keep taking your painkillers as your nurses explained prior to discharge
Your wound
You usually have your stitches, clips or staples removed about 7 to 10 days after your operation. Or if you have dissolvable stitches, they disappear over a few weeks.
Your nurses and surgeon check your wound regularly while you are in hospital.
Tell them if:
- You have any redness, pain or swelling
- It feels hot
- There is any fluid leaking
These are possible signs of a wound infection. Contact your nurse if the pain is not controlled or have any problems with your wound.
Holistic needs assessment
This screening tool is aimed to encourage professionals and patients to explore current problems and issues that may be affecting patients’ physical, psychological, social and spiritual well-being.
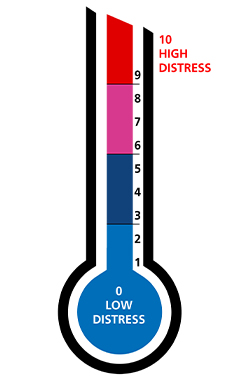
Social Concerns
- Coping with dependants
- Work or school
- Hobbies or leisure activities
- Housing
- Finances
- Travel
- Carer
- Relationships
Emotional wellbeing
• Sadness
• Fears
• Worries or anxieties
• Anger
• Alcohol or smoking or other drugs
• Unable to express feelings
• Feeling isolated
• Loss of dignity
• Forgetful or confused
• Stress
• Loss of control
Spiritual and religious concerns
- Questioning values and beliefs
- Sense of meaning
- Issues relating to dying and death
- Rest or activity
- Sleep
- Fatigue
- Tiredness
My appearance or body image
- Skin Dry or itchy or wound healing
- Swollen (limbs or abdomen)
- Weight changes – loss or gain
- Sexual problems
- Hair loss
- Other
Reduced independence
- Bathing or dressing
- Getting around
Toileting difficulties
- Constipation
- Diarrhoea
- Stoma
- Changes in passing urine
Physical symptoms
- Difficulties in communicating breathing
- Pain
- Temperature
- Change in sensation: hands and feet
- Seizures
- Other
Eating difficulties
- Indigestion
- Sores or painful mouth
- Nausea or vomiting
- Taste changes
- Swallowing difficulties
- Change in appetite
- Food preparation
- Other
- Any other factors
Exercise following thoracic surgery
Exercise after discharge from hospital
After your operation, your lung function should improve and your ability to exercise will gradually increase. However because of your lung condition you may have been unable to exercise for some time, so your increase in activity needs to be done gradually, to build your fitness slowly.
NHS Physical Activity Guidelines suggest people should aim for a minimum of 150 minutes of moderate exercise a week, however this may not be realistic immediately post operatively, it is a goal to aim for.
Regular exercise is proven to reduce the risk and severity of chronic disease as well as increasing your ability to recover from your surgery.
Moderate exercise includes activities such as
- Walking
- Riding a bike
- Yoga or pilates
The 150 minutes can be broken down as needed throughout the course of the week. Depending on your current levels of fitness it may be advisable to break the 150 minute total down into smaller, more manageable periods of exercise. If experiencing significant shortness of breath on exertion, pause, allow breathing to recover, then continue as able at a lower intensity if required.
Examples include:
7 x 20 to 25 minutes (one walk each day)
10 x 15 minute periods over the course of a week
The NHS website also has links to 24 instructor lead exercise videos ranging from 10 to 45 minutes duration. https://www.nhs.uk/conditions/nhs-fitness-studio/
Further information on how to increase your physical activity pre and post treatment can be found on the Macmillan “we are undefeatable” website https://www.macmillan.org.uk/we-are-undefeatable
Important
Post-op patients should avoid exercises involving loading through the upper limbs for the first 6 weeks
Pain
After lung surgery, it is normal to have some pain or discomfort. There are different ways it can be managed. Your nurse will assess you to make sure your pain is well controlled. This is important so you can do your breathing exercises. These exercises help reduce your risk of a chest infection.
Your doctor will give you painkiller tablets to take when you go home. You may have mild discomfort or pain in your chest. This can last for up to several weeks or months after surgery. Some people get new pain weeks or months after their operation. This is usually caused by nerves starting to repair after surgery. Tell your doctor or nurse about any new pain. They can check it and make sure you have the right painkillers.
Pain Score 0-10
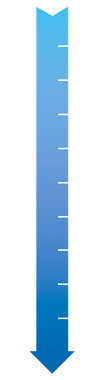
0 – No pain
1
2 – Discomfort
3
4 – Little pain
5
6 – Moderate pain
7
8 – Severe pain
9
10 – As much pain as could possibly bear
| Date and time | Pain score | Medication taken | Score after medication |
Help with prescription charges
The help you can get to pay for prescriptions is different across the UK.
If you need prescriptions for anything related to cancer or its effects, you can apply for a medical exemption certificate. You need to collect an FP92A form from your GP surgery.
This lasts for 5 years and can be renewed if you are still eligible.
Driving
Your doctor will tell you when it is safe to drive after your operation.
It can take about 4 to 6 weeks for you to be fit enough. At first, you may find the seatbelt presses on your wound and makes it sore. You can buy padding for seatbelts that may help reduce this.
Some car insurance policies give specific time limits for not driving after chest surgery. Check with your insurance company.
Contact us
Please contact the Advanced Nurse Practioners (Thoracic Surgery) if you have any questions or concerns.
Telephone: 01642 854532 , Monday to Friday, 7.30am until 6.00pm
Email: [email protected]
We are unable to respond to emails outside of normal office hours.
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact the patient experience department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the patient experience department of any special requirements, for example; braille or large Print.
T: 01642 835964
E: [email protected]