
Endoscopy
This leaflet describes the purpose of your procedure and what is involved for you. Please read this carefully before coming for the procedure so that you can be reassured about what will happen when you attend the Endoscopy unit.
Outpatient test – This leaflet should provide you with the all the basic information about the test. Patients will have been given the opportunity to ask any questions about the procedure when attending either an outpatient clinic appointment before the test or at the hospital pre-assessment visit.
Despite this, occasionally questions about the procedure remain. If you have any major concerns before then you should contact us using the contact details at the end of this leaflet.
In-patient test – The medical and nursing staff responsible for your care will be able to answer your questions regarding the procedure.
What is an ERCP?
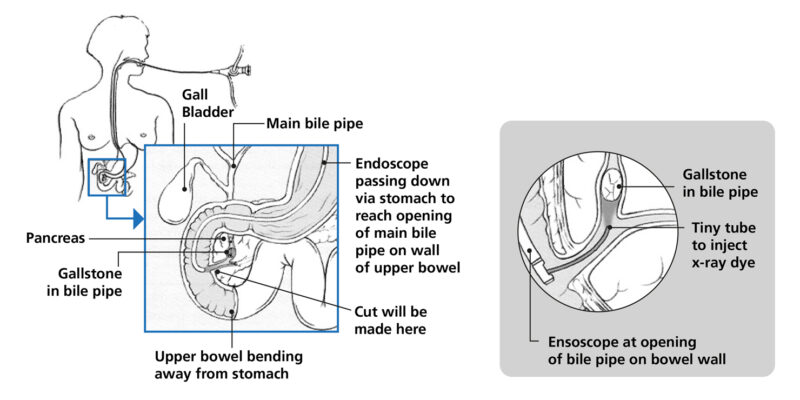
An Endoscopic Retrograde Cholangio-Pancreatogram (ERCP) is a procedure which allows the endoscopist (doctor performing the procedure) to gain access to the bile drainage system to deal with a variety of problems in this area.
To do this a flexible tube is passed down through the mouth – over the back of the tongue – to examine the gullet / swallowing tube (Oesophagus), Stomach and part of the Duodenum.
It is about as thick as your index finger. A small amount of gas is blown into the upper gut to achieve a clear view. When in the correct position in the duodenum a small cannula is passed into the bottom of the bile pipe. With fluoroscopy (x-ray) guidance the endoscopist can diagnose problems and offer appropriate treatment.
In some cases, it may be necessary to take biopsies (small samples of tissue), using tiny forceps or brushings, using a small pipe clean-like device to pick up cells from the biliary system. The samples are sent to the laboratory for analysis using a microscope. Taking biopsies or brushings is painless and very safe.
How may an ERCP help?
An ERCP is usually performed when someone has been identified to have a problem with the bile drainage system. This can often be because of an obstruction to the passage of bile (yellowy-green liquid produced by the liver). This can occur due to: –
- Gallstones in the bile drainage system.
- Abnormalities within the bile system (inflammation and narrowing or tumour growth).
- Compression of the bile duct from close by structures (such as with a tumour of the pancreas).
Bile duct problems can result in abnormal liver blood tests, jaundice (yellowing of the skin and eyes), abdominal pain, nausea and vomiting, or infective symptoms such as fever or shaking attacks (rigors). Sometimes an ERCP may be performed in someone without any symptoms but where there is a risk of further problems in the future, such as the risk of pancreatitis (inflammation of the pancreas gland) if stones are left in the bile duct.
Sphincterotomy (or internal cut)
When there is evidence of a gallstone or stones in the bile drainage pipe then a short internal cut can be made to the nipple like muscle structure (ampulla) at the bottom end of the bile duct. This then allows the stones to be removed by a balloon or basket. Occasionally the ampulla may need to be dilated with a balloon to help with this.
Stent (drainage tube)
When there is a narrowing or blockage in the bile pipe a small hollow tube (which can either be made out of plastic self-expanding metal can be inserted to allow the bile to flow normally. Such stent usually last for a number of months and may need to be replaced by a further ERCP at a later date.
If a stent is left in place you should expect to be given advice about when a further procedure is likely to be performed.
Is there an alternative?
An ERCP is usually only undertaken when previous imaging (ultrasound, CT or MRI scan) has defined that some type of treatment as required. An ERCP is only requested when there is strong evidence that a sphincterotomy (internal cut) or stent insertion for drainage will be required.
Surgery
In some circumstances, such as with a stone in the bile pipe, the only alternative type of treatment would be an open operation under a general anaesthetic. This would involve significant risk and recovery time.
Most ERCP patients can expect to go home the same day if a supervising adult is available. Even if a stone is removed from the bile pipe at ERCP it may be advisable for the gallbladder to be removed. A successful ERCP means that this is less urgent and the surgery is usually more straight forward.
Other causes of blockage can also be treated by surgery, but this is usually a very major undertaking. The requesting consultant will have considered this possibility and decided that this is not appropriate in in this case, often due to a person’s general condition, other medical problems all the underlying condition.
If you would like to discuss these possibilities further before consenting to ERCP, ask your doctor.
Not having an ERCP would limit your doctor’s ability to confirm the cause of your symptoms or condition and treat these effectively. You should discuss this very carefully with your doctor. If you decide against having your procedure, then please let the administrative team know so that the valuable appointment can be given to someone else.
What preparation is required?
When you get your appointment
Please review the medications you take well in advance of your procedure.
If you take any of the following medications then please contact the department using the details below.
- Anticoagulant medications to thin the blood (Warfarin, Dabigatran, Rivaroxaban, Apixaban or Edoxaban) or anti-platelet drugs (Clopidogrel, Prasugrel or Ticagrelor). Some of these need to be stopped before endoscopic procedures and some require additional treatment if they are to be omitted.
- If you are a diabetic on treatment with tablets or insulin. Special arrangements are necessary if you need insulin.
You should expect to be given the necessary instructions about what to do with these medications in the days before your gastroscopy at the time of booking your test. If you are not given this information, then please ask.
It will be helpful to the endoscopy team if you bring all your medications (or at least a list of these indicating the dose and how frequently they are taken) with you when you attend for your ERCP.
In the few days before your procedure
We usually arrange for you to have some blood tests performed within 72 hours of the procedure. These blood tests may be taken at the hospital or arranged through your GP practice. These tests are to ensure that you have an appropriate platelet count and clotting result so that the risk of any bleeding because of the procedure is not increased.
Occasionally these blood tests may be deferred until you attend for your procedure, but you would be advised of this in advance.
On the day of the procedure
To allow a clear view, the gullet, Stomach and Duodenum must be completely empty. This also makes sure that you do not vomit.
This means that you should not have any food for at least six hours before the appointment time for the ERCP. Clear fluid such as black tea, black coffee, squash or water can be taken up to two hours before the procedure.
After this time you must remain “nil by mouth”. This includes not chewing any gum.
Important
It is important to follow this exactly or we may not be able to go ahead with the test or the test may fail and you would have to wait again for another appointment.
What happens in the endoscopy unit?
Your appointment letter gives a time for you to arrive at the Endoscopy unit so that all the administrative and clinical checks can be performed before your procedure takes place.
Please note that although we do our best to work to appointment times the variable nature of the procedures undertaken in the endoscopy unit mean that you may experience a delay. Please be patient and bring something to occupy yourself during this time.
If you have not already done so, you will be asked to sign your consent form after you have had a final chance to ask questions and the clinician performing the test has ensured that the procedure remains appropriate for you.
We usually give patients a nonsteroidal anti-inflammatory drug suppository just before the procedure. This has some analgesic (pain relief) properties but also helps to reduce the risk of pancreatitis (inflammation of the pancreas) following an ERCP. You may also be given some antibiotic tablets to take early on the morning of your procedure or intravenous antibiotics may be given just prior to starting the ERCP.
Throat spray or conscious sedation?
An ERCP is not a pleasant experience and often lasts approximately 45 minutes. The vast majority of patients choose to have their ERCP performed with throat spray and conscious sedation.
Throat spray is a local anaesthetic spray. Throat spray has a bitter banana taste and is sprayed into the back of your throat before the procedure to numb the area. This numbness usually goes after about an hour. This helps during the procedure as the main discomfort with a gastroscopy is the sensation of the tube passing over the back of the tongue and down into the gullet.
With conscious sedation you will have a small plastic cannula inserted into a vein in your hand or arm. Medication can be given through this to make you relaxed for the procedure.
You will be conscious and awake throughout the test and may well have some awareness and memory of the test. Giving you sedation (often with the addition of analgesic, or pain relief medication) helps to ensure that this is not a distressing experience.
Having sedation means that you must follow the instructions below: (if not possible, please let us know).
- You must not go home alone, even by taxi. You must arrange an escort.
- You must be able to arrange for someone to be with you at home to supervise you until next morning.
- You must not drive any vehicle for 24 hours.
- It is also unsafe to operate any potentially harmful equipment or machinery and you should not sign any legal documents for the same period.
- If you were to take alcohol within the same period, it would have a more pronounced and unpredictable effect. You should avoid this.
What happens in the endoscopy procedure room?
- You will be asked to confirm your name and other details and the endoscopy team will make sure you and they agree that you have attended for the correct procedure.
- You will be asked to remove any false teeth, plates or dentures.
- If you are having throat spray then you will be asked to open your mouth and hold your breath for about 5 seconds whilst this is sprayed into the back of your throat. This taste can be an unpleasant bitter banana taste. After a few seconds you will be asked to swallow this. The numbness in your throat that this produces will fade after about one hour. This is a strange sensation and you may feel as if you cannot swallow. This is the desired effect due to the numbness but your ability to swallow remains intact.
- A mouth guard will be placed in your mouth to protect your teeth and gums as well as protecting the endoscope from damage.
- You will then be asked to lie on almost on your front with your left arm behind your back and facing towards the endoscopist on the right side. The endoscopy team will help to ensure you are positioned correctly before the procedure starts.
- A nurse will make sure of your comfort and dignity at all times.
- If sedation has been chosen, you will be given the intravenous sedative and pain relief medication through the cannula that has been placed in your hand or arm.
- A small tube will be placed in your nose to provide oxygen and a clip put on your finger to continuously check the oxygen level in your blood. The procedure will then be performed and you might be given more sedation, if required.
- Any excess saliva or secretions in the mouth during the procedure will be removed with a suction device. This avoids this partially obstructing your breathing or going into the lungs.
- A radiographer will be present in the room with the machinery to allow radiographic (x-ray) images to be taken during the procedure. Part of this equipment lies over the lower chest and upper abdomen during the procedure.
- If you want the procedure to be stopped at any time then raise your hand. The endoscopist will stop the procedure and if you are still unable to continue they will end the procedure as soon as it is safe to do so.
- During the examination your tummy may feel bloated and slightly uncomfortable as a small amount of gas is pumped into the Stomach to allow all the folds to be fully examined. This gas quickly disperses within a few hours.
- A number of photographs and radiological images are standardly taken during an ERCP procedure. These photographs are often added to the endoscopy report. In almost all cases you will be offered a copy of your report to take home. Separate copies will be sent to your General Practitioner and any other doctors involved in your care.
Are there any risks?
The risk from a straightforward procedure is small and the endoscopy team will do everything they can to keep you as comfortable and safe as possible. However, an ERCP is an invasive procedure and complications can occur.
- Rare serious complications are: –
- Perforation – A small leak can be produced in the wall of the small bowel. This is called a perforation and the risk of this is about 1 in every 250 patients. If this were to happen, hospital admission would be required and it might require an operation to mend it.
- Bleeding – There is a small risk of bleeding after obtaining biopsies from the gastrointestinal tract. Bleeding usually settles spontaneously but could require admission to hospital, a blood transfusion and a radiological intervention or operation to stop the bleeding in rare circumstances. This risk is about 1 in every 100 patients.
- Pancreatitis – Having an ERCP can cause pancreatitis (inflammation of the pancreas gland) as the pancreas gland is close to the bile drainage system. This seldom means more than some abdominal pain for 24 -48 hours (up to 1 in 12 cases) but this can be prolonged, severe and life-threatening in approximately 1 in 250 cases. In such circumstances prolonged admission, often necessitating a stay in the intensive care unit may be required.
- Death – The risk of death associated with an ERCP is approximately 1 in 250.
- There is a small risk of an allergic reaction to the sedative drugs that are administered (or less commonly the endoscopy equipment or other chemicals and substances used within the endoscopy unit) during the procedure. The endoscopy unit is a latex free environment.
- Excessive use of sedation could cause heart or breathing problems. If that happens, we might need to administer medicines to reverse the effect of sedation.
- It is unusual to have anything worse than a mild and brief sense of a sore throat and/or bloating.
- Damage to your teeth (including crowns and bridges), gums or lips is usually avoided by use of the mouth guard. Please alert the endoscopy team if you have loose teeth.
What happens after the procedure?
- Recovery after sedation is variable. You will be transferred to the recovery area with continued monitoring of your heart rate and oxygen levels.
- Most people are ready to leave the unit within 2-4 hours. Patients are asked to remain “nil-by-mouth” for 2 hours after the procedure and subsequently a drink is offered unless there is any concern regarding a complication.
- You should receive a copy of your report and a discharge instruction sheet. You should be informed about the next step in your care and how you will be informed of the results of any biopsies that have been taken. Usually this will either been by letter or at a forthcoming out-patient appointment.
- Please remember that if you have a stent in place your report or the associated discharge information should document when you could expect a further procedure for this to either be removed or replaced. If this is not clear, then please ask.
Contact us
If you require further information please contact us on:
Telephone 01642 282576 (Monday to Friday, 8am to 6pm)
Email: [email protected]
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]