
Respiratory
This leaflet is to help provide information about the drug Colomycin and how it can safely be administered. Including how to use and to maintain the equipment you need to help deliver the drug.
You have been prescribed a drug called Colistimethate Sodium known commonly as Colomycin®, this is an inhaled drug delivered through a nebulised system.
Why do I need this treatment?
Colomycin® is an antibiotic that is used to treat many different infections, it can be given nebulised, intravenously and intramuscularly. A nebuliser machine will turn the Colomycin® into a mist that you breathe in, it usually lasts around 15 minutes.
Studies have shown that regular treatment with inhaled antibiotics can reduce the number of bacteria in the lungs for certain conditions such as Bronchiectasis.
What are the benefits of using Colomycin?
Inhaled antibiotic therapy may:
- Reduce flare ups (exacerbations) of your chest condition
Improve your symptoms
- Improve the health of your lungs
Treat and kill certain bacteria in the lungs
Side effects
All medications come with the risk of side effects and it is our duty to inform you of these. The most common side effect for antibiotic therapy is chest tightness, because of this some patients are unable to use inhaled antibiotics.
To prevent chest tightness you will need a dose of nebulised Salbutamol first before you have the Colomycin. This will help to relax the muscles around the airways which should prevent any chest tightness. This will also help the Colomycin to get deeper into your lungs to help treat the infection providing a better benefit.
You will be given a Colomycin challenge first to ensure it is safe for you to take whilst monitoring your lung function health. This must be done under supervision by the Respiratory team in a clinical environment.
If there are no concerns, then you can be prescribed the inhaled antibiotic Colomycin.
If you do experience chest tightness around the time of administering the Colomycin at home, stop using it for two to three days and please inform the Marton Day Unit at James Cook University Hospital (see contact numbers on last page of information). Please also contact your GP if this continues as this could be caused by other medical conditions.
You will be shown how to use the equipment on the day of your trial. If a family member is going to be assisting you at home to administer the medication ensure they are present at your appointment for the explanation and demonstration.
Information for use of Colomycin®
First, you will need to take a dose of your nebulised Salbutamol solution before your Colomycin dose to prevent the chest tightness and help open your airways
- Doses are either 1 or 2 million units (sometimes written as 1Mu or 2Mu).
The respiratory team will decide which dose is suitable for you - Use twice a day
Space your dose 12 hours apart - Administered in a well ventilated room
Ideally without any other people or pets in the room.
When using the nebuliser some antibiotic will escape into the surrounding air via your mask or mouthpiece, because of this you should nebulise with the windows open and the door shut.
You can make you daily dose up in one go but your second dose must be kept in the fridge and used within 12 hours.
How long will I be on treatment?
If you are stable on Colomycin, you will need a minimum of 3 months. If it is effective, then you can expect to remain on this long term.
Inhaled Colomycin® and pregnancy
Do not use Colomycin® if you are pregnant as this can harm an unborn baby. Use birth control and inform your doctor if you are planning a pregnancy or become pregnant whilst on treatment.
Where do I get the equipment from?
The Marton Day Unit will supply you with:
- A nebuliser machine
- A 12-month supply of all consumables (masks, mouthpiece, tubing, nebuliser chamber and filters.
We will ask your GP to prescribe the Colomycin®, Salbutamol nebuliser solution and mixing solutions for the Colomycin powder for when you are at home.
Equipment required
- 1 Vial of Salbutamol nebuliser solution.
- Nebuliser mask for Salbutamol
- 1 Vial of Colomycin®
- 5ml Syringe
- 4mls of 0.9% Sodium Chloride for 2 million units
- 3mls of 0.9% Sodium Chloride for 1 million units
- Mouthpiece for Colomycin®
- Filters and tubing (filter pad should be changed at every use)
- Nebuliser machine.
Looking after the nebuliser machine
You should wipe your nebuliser machine with warm soapy water daily
- Dismantle your nebuliser equipment and clean under warm running water with liquid soap for 5 minutes, rinse thoroughly and leave to air dry
- You should put all parts including your mask and mouthpiece in boiling water. Boiled kettle water is suitable for at least 5 minutes once a day to disinfect. Please do be careful when removing the equipment from the boiling water, please ensure the water is cooled before removing
- You should change tubing once a year – you can obtain this from the Marton Day Unit at James Cook University Hospital
Please check individual manufacturers guidance on cleaning.
Instructions for use
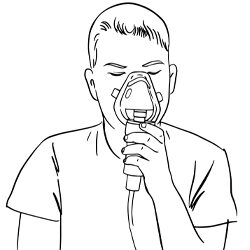
- Wash and dry your hands and assemble all necessary equipment. Squeeze the Salbutamol nebuliser solution into the hole of your nebuliser mask, or if you have a mouthpiece unscrew the mouthpiece off and place into the chamber and screw the mouthpiece back on. Then turn on your nebuliser machine and administer for 5 minutes until the solution has gone.
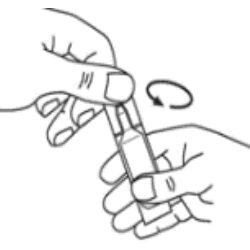
2. Gently tap Colomycin® vial on a hard surface to loosen powder.
3. Flip up the plastic cap from the Colomycin® vial.
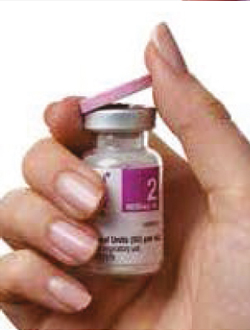
4. Remove foil seal by carefully pulling it away from the side of the vial, this should come
off in one piece.
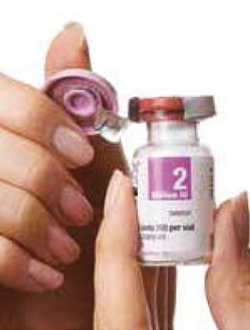
5. Remove the bung from the vial.
6. Twist the plastic cap off the Sodium Chloride ampule and draw out 3ml using the
syringe for 1 million units or 4mls for 2 million units.
7. Squeeze the Sodium Chloride from the syringe into the Colomycin® vial.

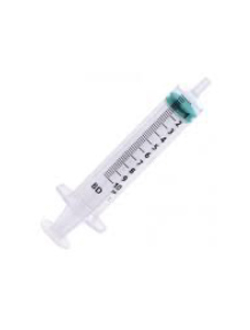
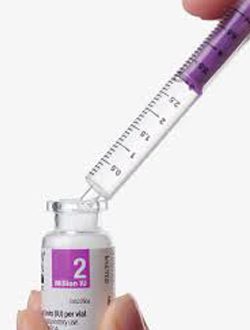
8. Replace the bung and swirl to mix. Avoid shaking as this causes frothing.
9. Remove the bung again and pour the contents of the vial into the nebuliser chamber.
Turn on your nebuliser machine and use as directed.


Contact us
If you require further information, please don’t hesitate to get in touch, the respiratory team will be happy to help.
- Marton Day Unit (JCUH site)
Telephone: 01642 854730, Monday to Friday, 08.00 until 18.30
Email: [email protected] - Respiratory Bronchiectasis Specialist Team
Telephone: 01642 854241, Monday to Friday, 08.00 until 18.00
Email: [email protected]
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]