Physiotherapy
This leaflet gives an overview of a neck dissection and what you can do to help your recovery
What is a neck dissection?
A neck dissection is an operation to remove lymph nodes; sometimes called lymph glands on one or both sides of your neck. This may be because your doctors know or suspect that there is cancer in the lymph nodes or there is a risk cancer may appear in them in the future.
A neck dissection can either be performed as part of a larger operation or as a stand-alone operation. It is an operation that is often performed as part of the treatment for head & neck cancer but can be part of other cancer treatments as well.
What are lymph nodes?
Lymph nodes (glands) are filters for the lymphatic system in your body. The lymphatic system is made up of lots of fine channels that drain tissue fluid. Lymph nodes respond to infection and try to stop it from spreading, sometimes this will cause the lymph nodes to swell and cause some tenderness.
With cancer cells, the lymph nodes filter them out and help in trying to prevent cancer cells spreading to the rest of the body. Therefore, lymph nodes with cancer cells in them need to be treated and removing them is one option.
The lymph nodes may have grown bigger than normal with the cancer cells or they may still be small (you may not be able to feel them) if there are only a few cancer cells within.
There are about 200 lymph nodes in your neck divided between the left and right sides.
Can I still fight infection when the lymph nodes are removed?
Yes. There are thousands of lymph nodes throughout your body which will still be there to fight infection.
What are the possible risks of the operation?
There are risks with any operation, so it is important that you are aware of them. Your surgeon will go through these risks with you as part of the consent process. Some operations are bigger than others, so not all of these risks will apply to everyone.
The list below describes some common risks associated with surgery, but this does not replace the discussion you will have with your surgeon about the risks relevant to your case. You may experience some of the following:
Bleeding and blood collection
Bleeding is not a common side effect but if significant bleeding occurs you may require a blood transfusion, if you are unable to receive blood products, please discuss this with the team. Occasionally further surgery is needed to stop bleeding.
Drainage tubes may be placed during surgery to drain off excess fluid to help prevent blood collecting in the wound, though in some patients this can be avoided. However, blood may collect under the skin and form a clot (haematoma).
If this occurs, it may be necessary to return to the operating theatre to remove the clot and change or place a drain. This is to help speed up healing and reduce the risk of infection
Infection
This could be a wound infection which may require a course of antibiotic. Risk of a chest infection can be reduced by deep breathing exercises and following your physiotherapist instructions. If you smoke, we strongly advise you to stop to help chest function.
Numb skin
Occasionally you may find that the skin around your neck dissection site may be numb after the surgery and this can last for months. This will improve over the following 12 months, but you should not expect the numbness to disappear entirely.
Swelling
It is not unusual to have swelling in the face and neck following this type of surgery. This will usually reduce and improve over several weeks following your operation. Some patients may have longer term swelling called lymphoedema, especially if they have had other treatments such as radiotherapy.
Chyle leak
Chyle is the tissue fluid which runs in lymph channels; occasionally, one of these channels (called the thoracic duct) leaks after the operation.
If this occurs, chyle can collect under the skin and you will need to stay in hospital until it stops. Sometimes it may be necessary for you to have another operation to seal the leak and you may need to eat a special diet.
Nerve damage or bruising
There are a number of nerves around the neck dissection site that may get damaged or bruised during surgery.
The aim is to avoid this but possible side effects include:
- Difficulty shrugging or lifting movement of the shoulder. If the accessory nerve is bruised it can stop working for several months. If this happens you may experience aching and some difficulty in moving your shoulder. This can make some tasks more difficult especially tasks requiring you to lift your arm above your head or reach behind your back.
You will be given some exercises to help you keep the muscles strong and active while the nerve is recovering. The exercises are included in this information leaflet.
Rarely, it is necessary to cut this nerve in order to remove the lymph nodes completely. If this is the case then these shoulder problems may be permanent; you will be referred for ongoing physiotherapy if the nerve is cut. - Lower lip and chin, one nerve helps move the side of the lower lip and if it is damaged or bruised you may find that the corner of your mouth will be a little weak. This is most obvious when smiling and sometimes affects drinking liquids. This is usually temporary but occasionally may be permanent.
- Tongue weakness, very rarely the nerve, which makes your tongue move, has to be cut or is bruised. In this case you will find it hard to clear food from the side of the mouth and may have some difficulty swallowing. It can affect your speech but most people can still produce clear speech even if this nerve isn’t working.
A speech and language therapist (SLT) will assess your swallowing and give you advice on how to cope with this should it occur. - Sometimes during the procedure, the lingual nerve which gives sensation to the side of the tongue may be stretched. As a result, there may be some tingling and numbness of the tongue which is usually temporary – it feels a bit like when an injection from the dentist is wearing off.
Will I have a scar?
A neck dissection will mean that you have a scar on your neck which will be visible; this will gradually fade over a few months.
What happens during the operation?
The surgical team will make a cut in the neck at the best place to remove the lymph nodes that need to come out. The lymph nodes will be peeled from around the nerves, vessels and muscles. Sometimes the nerves, vessels or muscles may need to be removed to safely remove the at-risk lymph nodes.
At the end of the operation one or more tubes (known as drains) may be placed through the skin. These remove any blood which may collect in the wound. Selected people may not need a drain if a special type of tissue glue is used.
What happens after the operation?
Every person has a slightly different recovery depending on the extent of the operation. Your face and neck may be quite swollen after the operation.
You will be seen by the doctors, nurses and other healthcare professionals as needed to review your progress and offer support and advice. The doctors and nurses will let you know when you can eat and drink after the operation. This may depend on whether you have had another operation at the same time.
You will need to stay in hospital at least until all the drains have been removed which usually takes between 1 and 3 days. This is not a painful procedure – the stitch is removed and the drain is removed at the bedside.
If your neck dissection is glued, please keep the area dry for 7 days after the operation then you can start to wash and peel fragments of the glue off as it lifts from the skin area. It may take a few days for all of the glue to lift.
If instead of glue your skin has clips or stitches, they will be removed seven to ten days after surgery. You will be advised whether this will be at the GP surgery or back at the hospital.
A discharge date will be discussed and decided depending on your recovery. The nurses on the ward will plan any extra care you may need after you leave hospital, such as visits from the district nurses if you need a wound dressing change.
Will the operation be painful?
Some discomfort is to be expected and is usually worse during the first few days. The nurses will be monitoring your pain regularly and will give you painkillers as necessary.
With any operation, it is normal to experience some pain, however, we aim to ensure that this is well controlled; please let the nursing staff know if you experience any problems with pain.
What will happen after I go home?
Once you are able to go home, we will give you an initial supply of medication and dressings if you need them. If you require further supplies, you will need to get them from your GP. Simple pain relief medication can be bought from the shops.
You will receive a follow-up appointment to check on your progress and to discuss the results of your operation. At this appointment we will discuss whether or not further treatment is needed.
If you have any questions, it may help to write them down as you think of them. It may also help to bring someone with you when you attend your outpatient appointments.
Will I need to have further treatment after my neck dissection?
This will depend on what is found when the lymph nodes are looked at under the microscope. It takes approximately 10 to 14 days to get the results. Your doctors may not know until then whether additional treatment is needed.
When can I go back to work?
This depends on the type of surgery you have had and if you need further treatment. You should discuss this with your surgeon. You should not lift heavy items for a minimum of four weeks after you go home.
Ask the nurses on the ward for a fitness to work certificate to cover you while you are in hospital. If you need more time off work you can get further certificates from your GP.
When can I drive?
Do not drive until your strength and speed of movement are back to normal, as you must be able to perform an emergency stop and turn your neck sufficiently for good visibility.
You should also make sure that you are not drowsy from any pain relief medication and that your concentration is good. Discuss this with your doctor, before driving if you are not sure.
Why should I exercise after?
After surgery it is important that you start to exercise by moving your shoulders and neck as normally as possible.
Movement may be reduced after surgery because of swelling, the position of any drains and stitches in your skin.
Gentle exercise will help to reduce swelling and help prevent stiffness in your neck and shoulders which may lead to pain.
What exercises should I do?
Exercises should be done gently and slowly, do not force movement. They should not cause pain but you may feel slight discomfort and a stretching sensation.
You may start your exercises once all of the drains have been removed so that you are able to move your neck freely. They can be started before all the clips or stitches are removed.
- Exercise should be done little and often.
- Aim to complete each exercise three to five times a day.
These exercises can be completed in either sitting or standing.
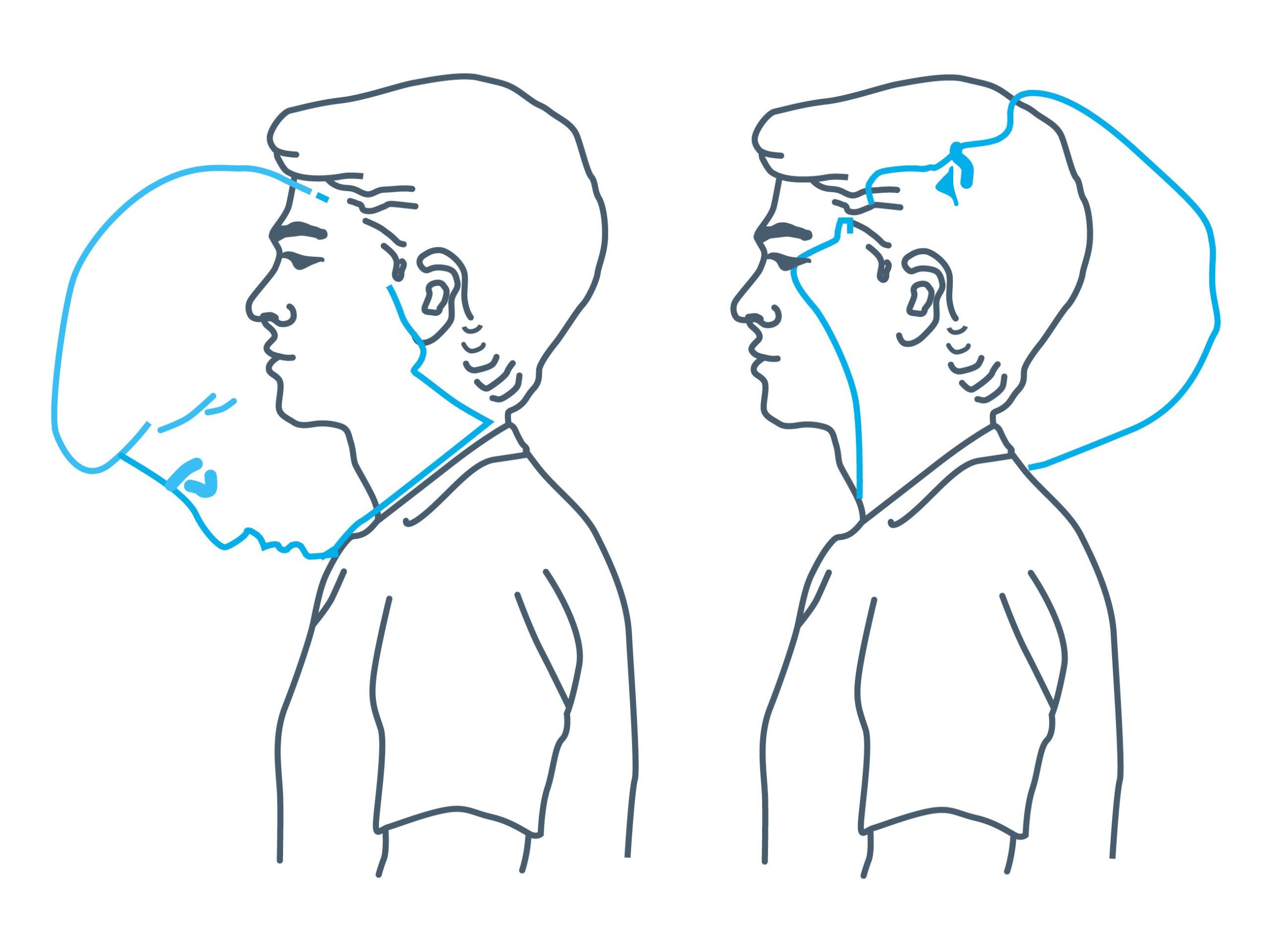
Neck exercises
Exercise 1: Tilt your head down towards your chest, hold for 5 seconds until you feel a gentle stretch at the back of your neck. Return to the centre.
Now look up towards the ceiling until you feel a gentle stretch, hold and try to keep your lips closed.
Repeat 5 times in each direction.
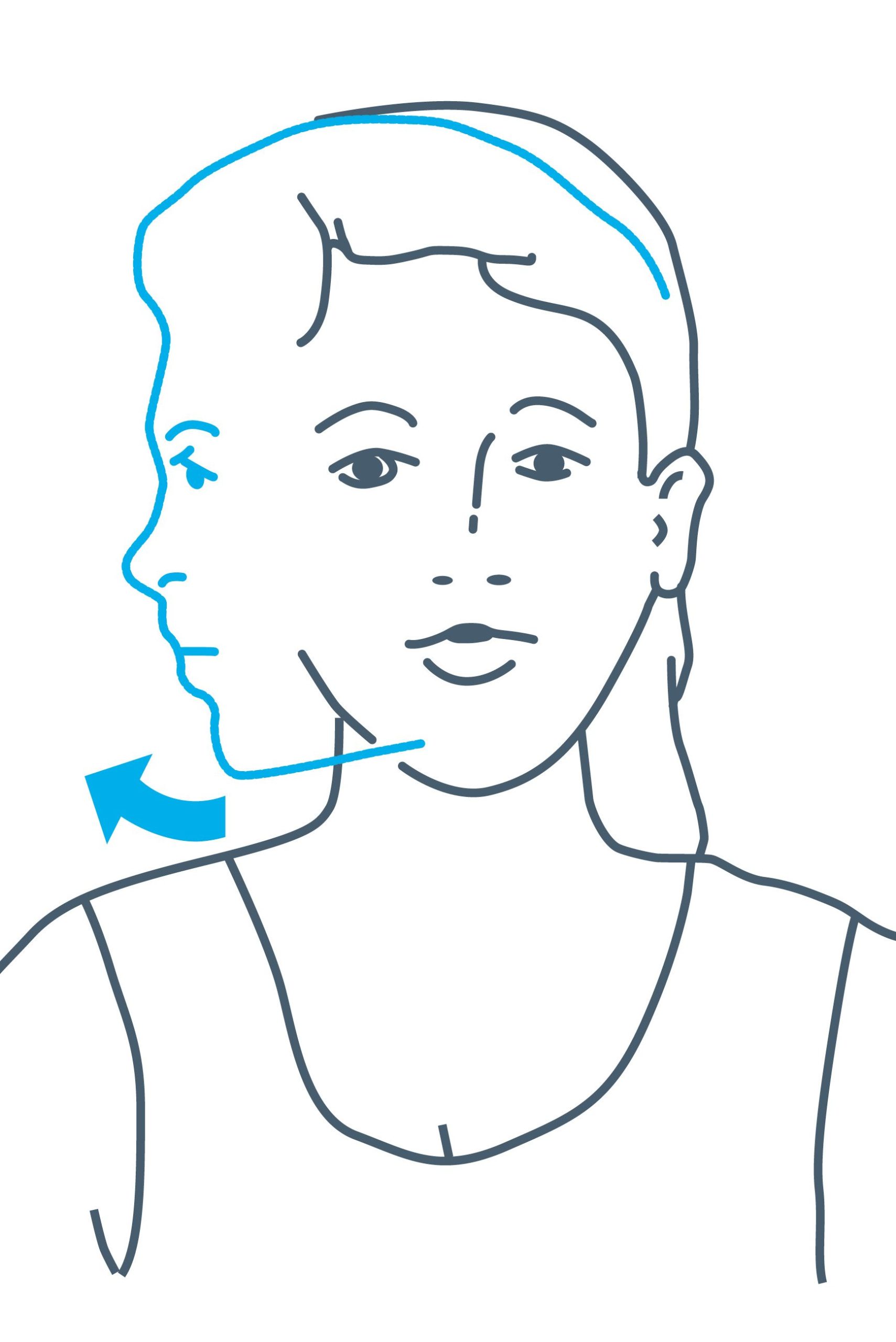
Exercise 2: Bend your head to the side, trying to bring your ear as close to your shoulder as you can.
Keep your shoulders relaxed. Hold for 5 seconds then return to the centre.
Repeat on both sides, 5 times each direction.
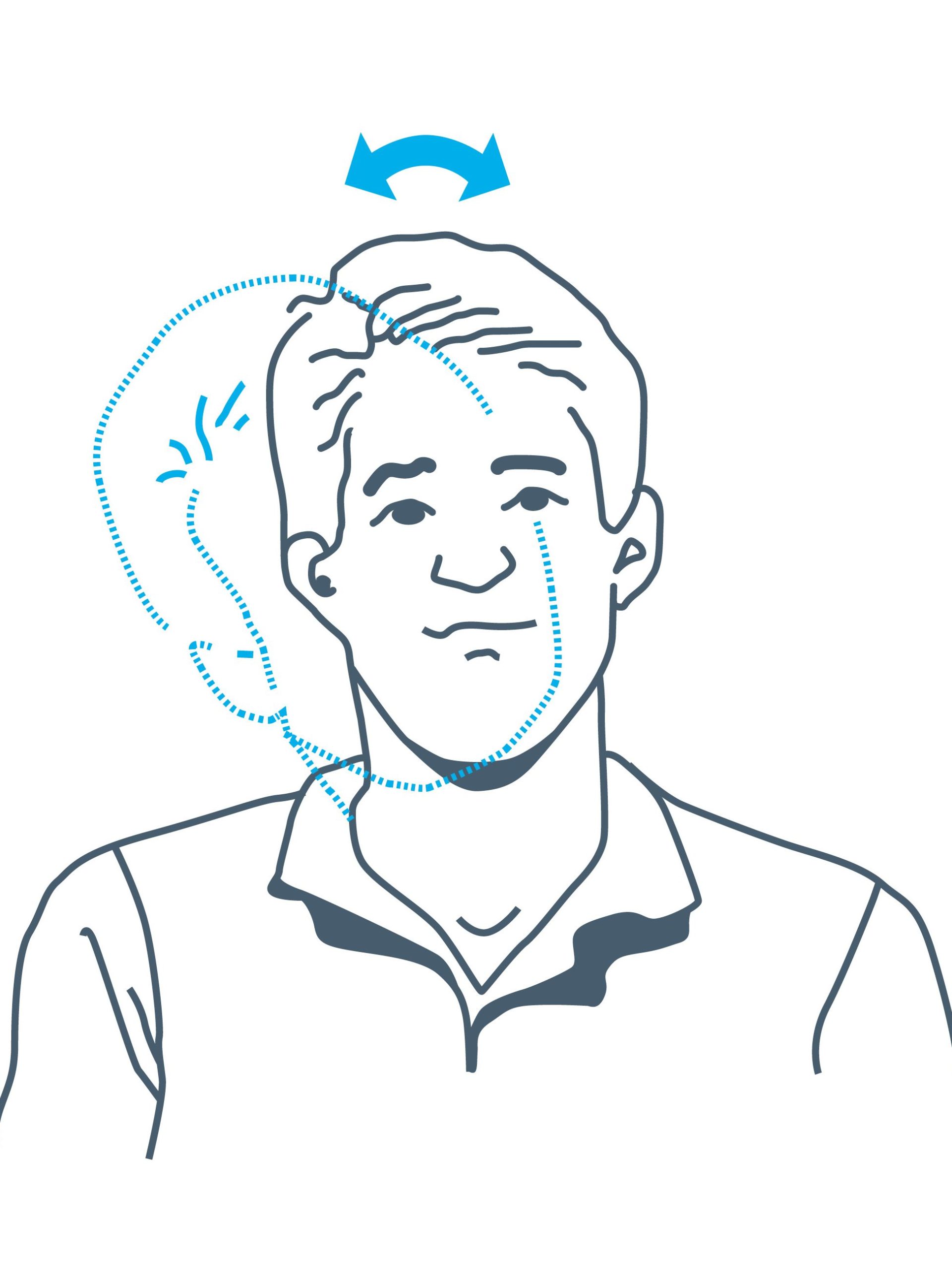
Exercise 3: Turn your head towards one side as though your shoulder, keeping your chin at the same heights and moving within comfortable limits.
Return your head to the centre and repeat on the opposite side.
Repeat 5 times on each side.
Shoulder exercises
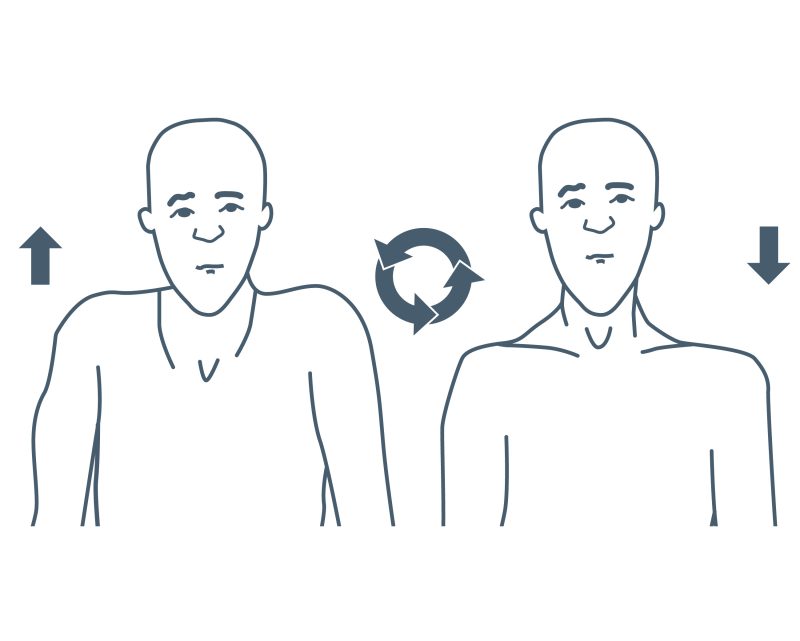
Exercise 1: Lift your shoulders up towards your ears as though shrugging your shoulders, hold for a few seconds and gently lower as far as you can, then relax.
As you feel more confident with this exercise; lift your shoulders upwards, gently roll them backwards as though opening up your chest.
Repeat each exercise 5 times.
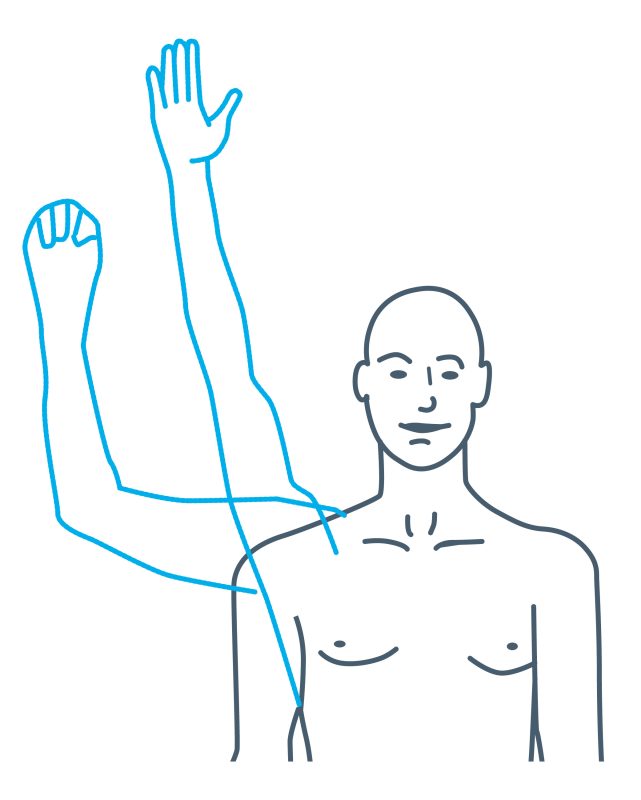
Exercise 2: Lift your arms up one at a time; let your thumb lead the way. Only go as far as is comfortable, gradually increasing the movement with time. Repeat 5 times on each arm.
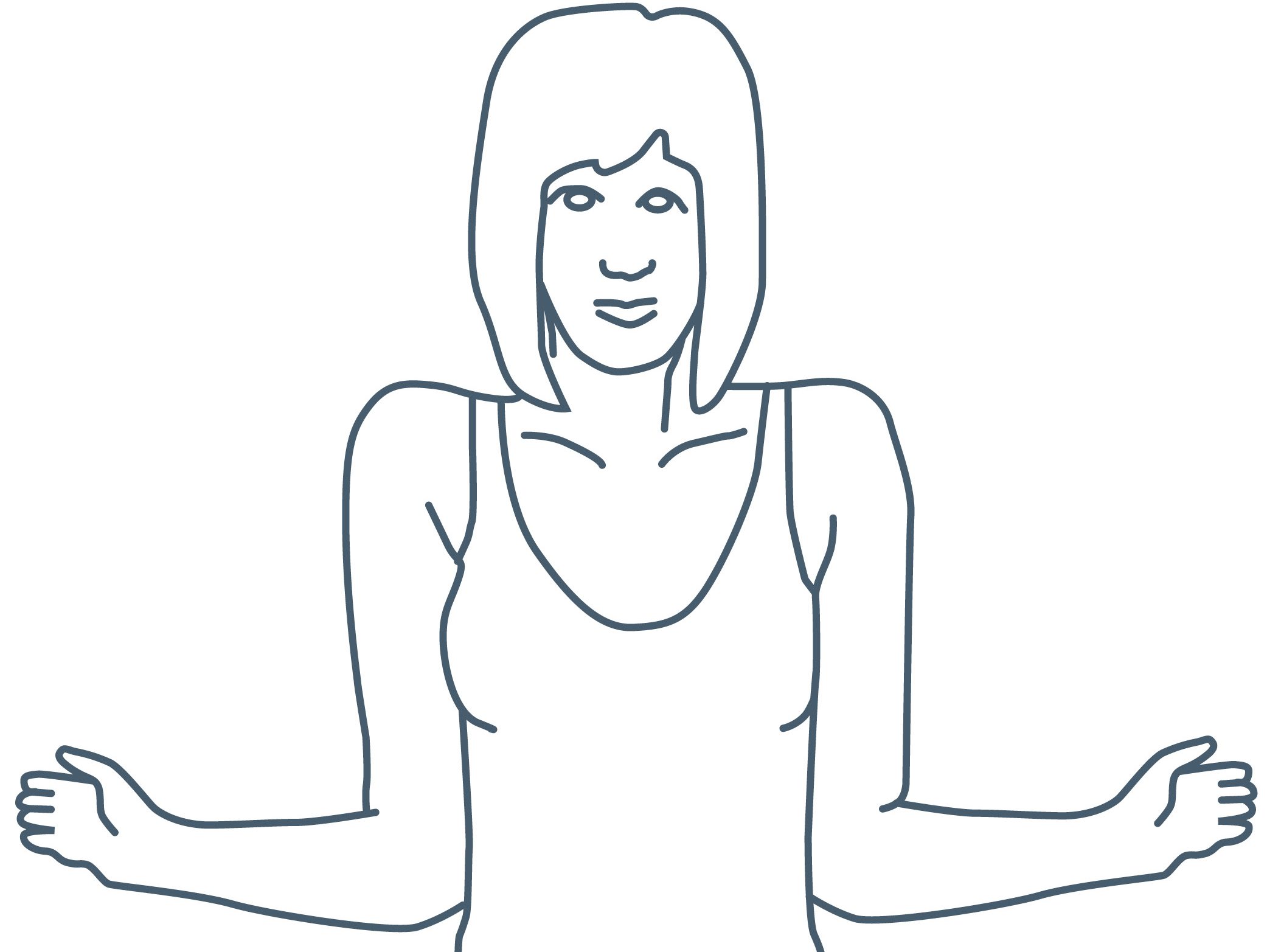
Exercise 3: Bend your elbows and keep them tucked into your sides.
Gently move your forearms outwards and back again.
Repeat 5 times.
Scar massage
Massaging the scar can help to improve the size and appearance of your scar, and the range of movement at your neck. Massage should only be started once the wound is fully healed (when there are no scabs or open areas) and you have finished any radiotherapy.
- Use a moisturising cream (non-perfumed if you are concerned about skin irritation)
- Gently press on your scar, moving it and the surrounding tissue with your fingers
- Make small circles, moving the skin over the tissue underneath, rather than rubbing on the skin surface
- Massage for about 5 minutes, 2 to 3 times a day
If you notice any change in the appearance of your skin, for example it becomes more red, painful or starts to ooze, stop the massage and speak to your GP or consultant.
Lymphoedema
After your operation, you may be more likely to develop swelling (known as lymphoedema) around your face and neck, where the lymph nodes were removed.
For further information and advice on how to manage lymphoedema, please speak to your Specialist Nurse.
Additional information can also be found at:
Returning to normal activities
Provided there are no problems with wound healing, try to return to normal activities (such as washing and dressing yourself) while in hospital.
You can start to do some light domestic chores as soon as you go home. Try to build up to longer/heavier tasks gradually over the next 4 to 6 weeks.
For the first 2 weeks after your operation, try to avoid heavy activities such as hanging out wet washing and lifting anything heavier than a full kettle, for example shopping bags or children.
Contact us
If you require further information please contact:
- Head & Neck Specialist Nursing Team
Tel: 01642 835702
Email: [email protected] - Speech and Language Therapist Team
Tel: 01642 854039
Email: [email protected]
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]