
Physiotherapy
Pelvic Girdle Pain (PGP) is a pregnancy related term used to describe pain experienced in the front and, or back of your pelvis. As many as one in five women may be affected by this condition.
Women may experience a variety of symptoms ranging from mild discomfort to severe pain which interferes with daily life.
Signs and symptoms of PGP
The diagrams below show the bones and joints that make up the pelvic girdle. PGP commonly involves discomfort felt over the pubic bone at the front – formerly known as Symphysis Pubis Dysfunction (SPD) – or across one or both sides of the lower back.
Pain may be experienced in all or some of the darker shaded areas shown on the diagrams.
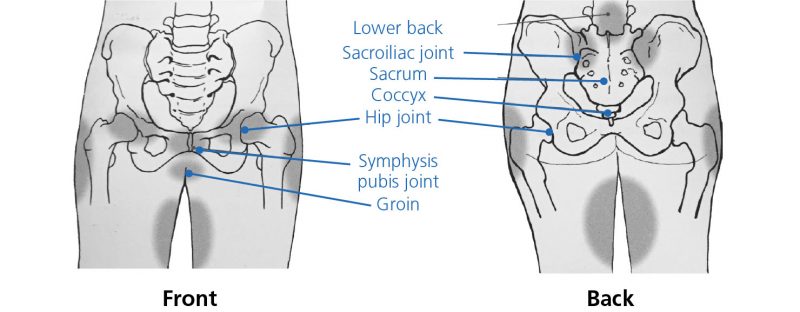
The discomfort may be described as an ache, a shooting pain or the feeling of being ‘kicked’.
Other symptoms of PGP may include pain and difficulty when walking or other movements involving standing on one leg such as climbing stairs, dressing or getting in or out of the bath.
It may also be painful when moving your legs apart, for example; getting in and out of the car or turning over in bed. Clicking and grinding may be felt or heard in the pelvic area.
Causes of PGP
PGP is most likely the result of a combination of different factors including:
- Underlying damage from a previous injury to the pelvis.
- Uneven movement of the pelvic girdle joints (sometimes due to pregnancy hormones).
- Weakness and poor coordination of the muscles surrounding the pelvis causing instability.
- Work or family demands including activities involving prolonged standing, twisting, pushing or pulling, heavy lifting.
- Increased mobility of other joints (hypermobility conditions).
- Previous traumatic labours involving excessive pushing or parting of the legs especially when laid flat on the back.
Management of PGP
In order to manage your condition as effectively as possible, a combination of approaches may be necessary including general advice and pain relief from your GP and physiotherapy assessment and treatment
You can help to manage the symptoms of PGP yourself by applying some of the following general advice.
Try to
Be as active as possible within pain limits and avoid activities that make the pain worse. Moderate exercise is good for you and your baby. Walk slowly with a shorter stride to reduce pain, wear flat supportive shoes. Swimming can be of benefit but with gentle breaststroke legs or vary your strokes. Avoid high impact exercise such as running, racquet sports and aerobics.
Ask for and accept help from your partner, family and friends with household tasks when necessary.
Rest when you can – you may need to rest and sit down more often sit down to get dressed and undressed.
Avoid standing on one leg.
Avoid standing to do tasks such as ironing, try sitting down.
Try to keep your knees together when getting in and out of the car. A plastic or silk carrier bag on the seat may help you to swivel.
Try to:
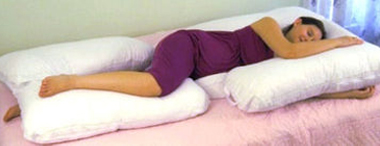
Sleep in a comfortable position, for example, lie on your side with a pillow between your legs.
Try different ways of turning in bed, for example; turning under or turning over with your knees together and squeezing your buttocks.
Roll in and out of bed keeping your knees together.
Take the stairs one at a time,try going upstairs leading with your better leg and downstairs lead with the more painful one or go upstairs backwards or on your bottom.
Plan your day – bring everything you need downstairs in the morning and have everything to hand such as drinks and snacks.
If using crutches have a small backpack to carry things in.
If you desire sexual intercourse consider alternative positions, for example, lying on your side or kneeling on all fours.
Try to AVOID activities that increase your pain:
Standing on one leg, for example; shaving in the shower.
Bending and twisting to lift or carrying a toddler or baby on one hip.
Crossing your legs, sitting on the floor or sitting twisted.
Stairs, walking up steep slopes or on uneven surfaces, for example; fields, cobbles, the beach.
Sitting or standing for prolonged periods.
Lifting heavy weights (shopping bags, wet washing, vacuum cleaners, toddlers).
Pushing or pulling heavy objects like supermarket trolleys.
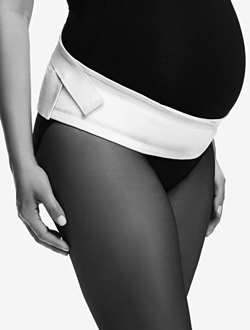
Physiotherapy treatment aims to improve muscle function, improve posture and stability, aid movement and relieve pain. It may include advice, strengthening exercises and exercises in water (hydrotherapy).
If indicated, you may be provided with equipment such as support belts or crutches.
You should continue with any advice and exercises throughout your pregnancy and for at least three months after the birth of your baby by which time it is most likely that your symptoms will have settled.
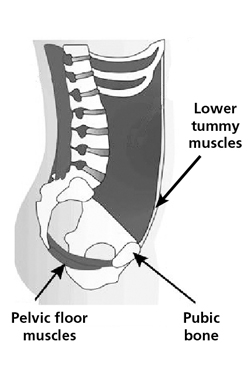
Simple exercises to increase stability of the pelvis
During pregnancy the tummy muscles stretch as the baby grows and the resulting weakness can reduce the support they give to your pelvis and back.
A simple exercise to strengthen these muscles is to regularly tighten your lower tummy gently as if you are trying to do up the zip on slightly tight trousers.
You should feel your bump lift slightly as the muscles tighten. Don’t hold your breath.
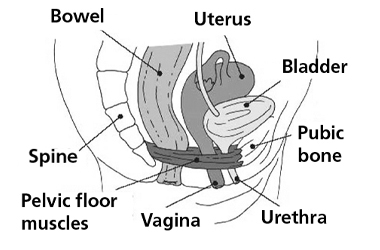
The pelvic floor muscles are other very important muscles in supporting the pelvis. They form the ‘floor’ at the base of the pelvis and help control your bladder and bowel. During pregnancy, the increasing weight of the baby may weaken the muscles so it is vital to regularly exercise them.
Imagine you are trying to stop passing wind and at the same time trying to stop yourself having a wee.
You should feel the muscles tighten around your back passage and front passage and hopefully feel a lift as you ‘tuck up’ the area between the back and front passage.
Try to do
- 5 to 10 long squeezes (up to 10 seconds hold with 4 seconds rest between each one) and 5 to 10 quick 1 second squeezes.
Don’t hold your breath or clench your buttocks. At least three times a day is the ideal.
It can also be really helpful to tighten both the lower tummy and pelvic floor muscles during movements that strain your pelvis or increase your pain for example, turning in bed, sitting to standing, bending or lifting and when doing the stairs. If you practice this regularly it will become an automatic reaction.
Implications of PGP during labour
Most women with PGP are able to have a normal vaginal delivery and a caesarean section is not normally recommended. However, you can discuss this with your midwife or doctor.
During labour think about birthing positions that are comfortable for you. Upright and forward-leaning positions are preferable as they reduce strain on your pelvis and gravity can better assist the labour, for example, kneeling on all fours or over a ball, beanbag or standing. Try to change positions regularly.
Avoid lying on your back as it may increase pain and slow labour. Squatting may also be uncomfortable.
It is extremely important not to place your feet on the midwife or your partner’s hips when pushing in labour as it may put too much strain on your pelvis and aggravate your symptoms following delivery.
During pregnancy you may find that you have some restriction in how far you can move your knees apart due to PGP. So before labour starts it can be useful to measure how far apart your knees can separate without pain (your pain free range) when lying on your back or sitting on the edge of a chair with your feet apart.
You should take care to keep your legs within your pain-free range of movement as much as possible during labour and birth to protect your joints.
Where you need forceps, ventouse delivery or stitching, care should be taken by the midwives and doctors when placing you in the lithotomy position (i.e. in stirrups), to lift and part your legs both at the same time, and try not to exceed the pain-free range of movement.
PGP after the birth
Many women find that their symptoms settle quite quickly after the birth but it can take several months for the tummy and pelvic floor muscles to recover and for the hormonal effects on the joints to subside.
Breast-feeding does not interfere with recovery from PGP as different hormones are involved.
Whether or not you have pain postnatally, it is essential that you continue with the same advice and exercises you followed during pregnancy, especially lower tummy and pelvic floor exercises, for at least three months. Gradually increase your activity levels as pain allows.
Future pregnancies
Some women may experience PGP again during a subsequent pregnancy. However, if it is well managed, the symptoms may not be as severe.
There is no particular evidence that time between babies affects the likelihood of further PGP but it is advisable to give your body at least 12 months to fully recover before trying to fall pregnant again.
It is worth considering whether your toddler will be able to walk while you are pregnant, to reduce the strain on your joints if you do have pain during any future pregnancy.
Useful information
Pelvic obstetric and gynaecological physiotherapy website: thepogp.co.uk
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]