Macmillan Cancer Support
What is it?
This leaflet is about ‘squamous cell carcinoma’ which is one type of cancer that affects the tongue base (back of tongue) and tonsil – sometimes together called throat cancer.
This area is known as the oropharynx in medical terms.
Treating tongue base or tonsil cancer
Treatment options can include:
- Surgery
- Radiotherapy (with or without chemotherapy)
- Combination of surgery and radiotherapy (with or without chemotherapy)
Not everyone is able to have all of the treatments. This depends on how the cancer looks on the scans, biopsies and how fit you are as a patient.
Where is this area?
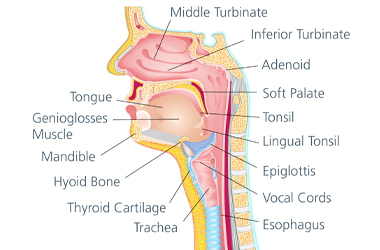
1. Non-surgical treatment
Radiotherapy (strong focused x-ray treatment) is a way of dissolving the cancer in the tongue or tonsil and neck glands.
In order to give radiotherapy you must be in the same position each day on the treatment couch, in order to do this you will have a plastic mask made that will fit tightly over your head and shoulders. You will still be able to breathe through holes in the mask.
The treatment machine will move around and deliver the radiotherapy but you will not
see or feel the treatment during this time.
Each treatment takes about 20 minutes, but you will be in the department around an hour each day. Over time the side effects of the radiotherapy treatment build up.
Side effects can include:
Tiredness
Skin reactions and soreness
Mouth and throat soreness
Taste changes
Thick and sticky saliva
Swelling difficulties
Nutrition
To help you keep strong and stop you losing weight we may recommend a feeding tube into your stomach (a PEG tube) or a NG tube (through your nose). If a PEG is required, you will meet the gastroenterology team and PEG nurse who will explain this procedure in more detail with you.
This is an overnight procedure and you will be shown how to care for this tube prior to going home by a specialist nurse.
You will be given a special liquid diet and this will be delivered to your home from a company called Nutricia. Your PEG tube will only be removed once it has been decided with the team that your swallowing has recovered and your weight is stable.
If an NG tube is recommended this will be inserted in the outpatients department when needed.
Dental
You may also need some or all of your teeth removed (depending on how healthy they are). Dental extractions are to help prevent long term problems with the jaw bone.
Usually these extractions are performed before you start your radiotherapy.
Your dentist may be involved in this treatment and you may need to find a dentist to arrange denture construction. We recommend not wearing any dentures for at least 6 months after radiotherapy.
Chemotherapy
Chemotherapy maybe used to help the radiotherapy work better in those who are fit and under the age of 70. The chemotherapy works by making the tissues more sensitive to the radiotherapy, this also means the side effects increase.
Chemotherapy is given through a drip in the arm once a week, every week throughout the six weeks. You will be in the department for the whole day having this drip.
Chemotherapy can make you feel sickly, but anti-sickness drugs are given.
It can affect your blood and you could become anaemic needing a blood transfusion.
The most serious side effect, is a drop in the white blood cells which fight infection. You will be given clear instructions of what to look out for and a 24 hour helpline number to call for advice and help.
Important
It is important that you follow the instructions given as infections after chemotherapy can be life-threatening if ignored.
You will be reviewed weekly to support you with your side effects from treatment.
Around 6 weeks after finishing treatment you will return to the Ear, Nose and Throat (ENT) department or Oral and Maxillofacial (OMFS) department for your follow up appointment.
You will get examined in clinic and you may get a repeat PET CT scan at 12 weeks after your last radiotherapy treatment to help see how the cancer has responded.
Some people need some surgery to remove glands in the neck that haven’t fully gone away with the radiotherapy (see below about neck surgery). This is not needed in everyone but if you do need it, then it is thought to be part of the full treatment and not a failure of treatment.
2. Surgical treatment followed by radiotherapy
If your cancer is suitable for surgery this will be in two parts
- To treat any neck glands that may contain cancer
- To remove the cancer in the tongue or tonsil.
- Usually you will need a smaller dose of radiotherapy after the surgery to treat any microscopic cells (see below).
Neck surgery
The neck glands that contain or might contain cancer in the neck need to be removed.
Surgery to remove the glands in the neck is called a neck dissection. This can take between 1 and a half to 4 hours. This can be done through a skin fold incision which is well hidden. There are nerves in the neck that need to be looked after when removing the glands.
Your surgeon will do their best to leave these nerves undamaged but the consequences of damaging the nerves are:
- weak movement of the tongue
- weak angle of mouth
- altered taste on the tongue
- numb neck or ear skin
- weak and heavy shoulder
In preparation for the surgery to your tongue and, or tonsil you will have one of the neck arteries tied off to decrease the risk of bleeding. You don’t need this artery and it is safe to have it tied.
Other risks of surgery include:
- infection
- fluid leak
You may have a drain put into the skin to take away any fluid or blood, when the drainage is minimal the doctors will decide to remove the drain. This is a simple procedure performed by the nurses on the ward.
When the drain is taken out you should be able to go home – this can vary from 1 to 5 nights in hospital.
You may have stitches, staples or wound glue to close the skin. If you have wound glue then you still have stitches under the skin for strength, they simply dissolve.
If you need any teeth removed, they are often removed at the time of your neck surgery and you may need painkillers as the gums heal.
Tongue or tonsil surgery
Surgery to remove a tongue base or tonsil cancer can be done via the laser or a robotic surgery. This involves removing the cancer and a small rim of normal tissue. Surgery is all done through the mouth and takes between 1 and 3 hours.
There will be a raw, sore area where the surgery is performed. This soreness can affect your eating and drinking and it is common for patients to require a feeding tube up their nose (nasogastric tube) to ensure adequate nutrition and hydration until the raw area gets better. This may be a couple of days up to a few weeks.
The main risk is bleeding (which is why the artery in the neck will be tied off).
Once you are eating and drinking or able to manage the feeding tube yourself you will be able to go home and be seen in a couple of weeks with your results.
Additional treatment after surgery
The radiotherapy (with or without chemotherapy) varies depending on the results from your surgery. Radiotherapy is often given in a lower dose. If this is the case a PEG feeding tube may not be necessary, or the option of a feeding tube through your nose (nasogastric tube) may be discussed.
Sometimes, the features of your cancer mean that you may require the full chemo-radiotherapy treatment as described above. If this is the case you will need either a NG or PEG feeding tube to get through this. The side effects are as written in the previous section.
You may or may not need a PET CT at 12 weeks after treatment. Your doctor will tell you if it is needed. It is less likely to be helpful after surgery.
Trials
You may be offered the option to enter into a clinical trial
These trials are to help us to find out improved ways to treat head and neck cancers
We only enter in trials that we feel are safe for you to be in
If you choose not to be in a trial no-one will mind
Follow-up
You will be followed up in the cancer clinic for 5 years, initially every 4 to 6 weeks, then less often as the years go on. You will be examined every time and usually you will not need any scans.
If you have any worries between appointments, you can see your GP or contact the specialist nurse and you may be brought in for an earlier appointment if needed.
After 5 years, as long as you are not smoking or drinking excessively you will be discharged as cured from your cancer.
Further information
Please visit our website for more information or ask your Clinical Nurse Specialists.
Contact us
If you have any concerns or questions, please contact the MacMillan Head and Neck Clinical Nurse Specialists on:
Telephone: 01642 835702, Monday to Friday – 09:00 until 17:00
Email: macmillan-head&[email protected]
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]