Tissue Viability Team
The purpose of this leaflet is to provide you and your carer information on pressure ulcers, how they develop and how to prevent them.
- A pressure ulcer is also known as a pressure sore or bed sore.
- They are areas of damaged skin or tissue that develop when there is constant or repeated pressure to your skin and tissue underneath.
- The skin may change colour or be broken, wounds may be shallow or small but can quickly become larger or more deep if pressure is not relieved.
- Pressure ulcers tend to happen over your bony areas but can occur under medical devices or if clothing or bedding is ill fitting or rucked up.
Common sites for pressure:
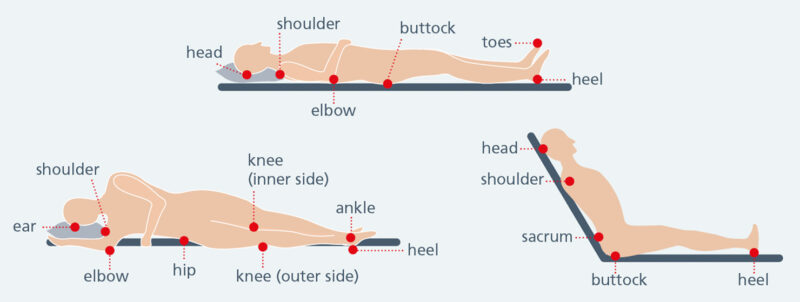
Who is at risk?
Anyone can get a pressure ulcer, particularly people with poor mobility who spend a lot of time in bed or chairs. Older people are more likely to develop pressure ulcers.
Also, people with:
- Diabetes or neuropathy
- Poor circulation
- Poor appetite
- Serious illness or major surgery
- Respiratory disorders
What are the signs and symptoms to look for?
-
Do you have any problems with movement?
-
Do you have poor circulation?
-
Do you have any pain on any bony areas? (For example, bottom, heels)
-
Is your skin often moist? (For example, sweating or incontinence)
-
Have you ever had a pressure sore before?
-
Do you eat well or experienced weight less recently?
-
Do you drink enough water (6 to 8 glasses a day)?
If you have answered YES to any of these questions you may be at risk of developing a pressure ulcer.

I have developed a pressure ulcer, what should I do?

Seek help as soon as possible from your doctor or nurse.
Follow the prevention advice in this leaflet.
What can I do to help?
- Check your skin regularly and report any signs to nursing team or carer.
- Keep moving – change position as much as possible. If in bed, alternate between back and sides
- When sitting in a chair relieve pressure on your bottom regularly, stand if you are able to, or shift weight from side to side
- Elevate heels
- Ask for help if required
- Manage moisture – keep skin clean and dry
- Regularly moisturise skin focusing on areas such as heels and elbows
- Eat well – high protein diet helps to repair damaged skin
- Eat a diet rich in vitamins and minerals
- Drink plenty of fluids
Pressure ulcers can be caused for many reasons
- Pressure: the weight of your body pressing down on your skin
- Shear: the layers of your skin or deeper tissue sliding over one another, for example, if you slide down or are pulled up a bed.
Pressure ulcers can develop very quickly if you are unable to move, sometimes within a few hours.
Whilst you are under our care at South Tees Trust we aim to:

- You will be assessed by a registered nurse or Assistant Practitioner to see if you are at risk of developing or have previously had a pressure ulcer. This will happen at the time of your admission and at regular intervals throughout your admission.
- If at risk or have a pressure ulcer, you will be assisted to or advised to regularly change position and move around.
- May require different equipment for example, mattress, chair cushion.
- You may see specialist teams such as Tissue Viability Nurses.
- You may require assessment from dietician for dietary advice.
- Regular wound dressings to aid healing.
Advice provided by your healthcare professional
How often should I move?
| In Bed: | In Chair: |
What equipment is recommended?
| Mattress: |
| Setting: |
| Cushion: |
| Skin cleansing: |
| Heel offloading advice: |
| Other advice: |
Contact us
For further information please contact the Tissue Viability Team:
Telephone: 01642 854103
Available Monday to Friday, 8.00am until 16.00pm
Email: [email protected]
You can call 24 hours a day, 7 days a week – please leave answerphone message.
All calls are returned during office hours.
Patient experience
South Tees Hospitals NHS Foundation Trust would like your feedback. If you wish to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Department who will advise you on how best to do this.
This service is based at The James Cook University Hospital but also covers the Friarage Hospital in Northallerton, our community hospitals and community health services.
To ensure we meet your communication needs please inform the Patient Experience Department of any special requirements, for example; braille or large print.
T: 01642 835964
E: [email protected]