Dry and cracked heels
Dry and cracked heels are generally caused by lack of moisture in the skin which can be worse when wearing open backed shoes such as sandals.
Treatment and prevention
- File the hard skin once or twice weekly with a foot file when the skin is dry. The easiest way to do this is to sit on a chair and hang your arm down and then bring your foot back to meet the file
- Cream your feet daily after a bath or shower with a thick moisturising hand or foot cream.
- Consider wearing socks or stockings or closed in shoes even in hot weather if you find the dry skin is worse or the skin cracks.
- Continue to apply the cream daily when the skin is better to prevent recurrence.
Athlete’s foot
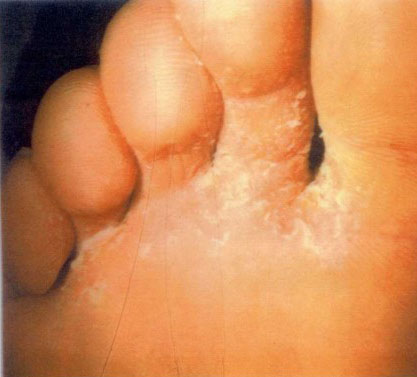
It has an appearance of redness and flaking with small red spots and is usually itchy. The ideal living conditions for Athletes foot are a place that is warm, damp and dark.
For this reason it is commonly found between the toes where the skin is moist but it can affect, or spread to, other areas of the foot.
People with diabetes, sweaty feet or a reduced immune system are more prone to suffer with this condition.
Prevention
- Dry carefully between the toes after bathing.
- Allow shoes and boots time to dry before wearing again. It is less likely that the infection will live in your shoes if they are properly dried.
- If possible, alternate between shoes especially if you work long shifts or work in a very hot environment.
- Make sure socks are washed regularly.
- Avoid putting extra moisture such as cream between your toes.
- Try to allow your feet some time to air each day.
- Wear cotton or wool mix socks to allow moisture to evaporate.
Treatment
There are many preparations available from your GP or Pharmacist to treat Athlete’s foot. It is important to follow the directions on the packet carefully.
We advise that you continue to treat your feet for a fortnight after you think the condition has cleared. This is to lessen the chance of re-infection. It is also important to follow preventative measures as listed above.
Verrucae (Plantar Warts)
We only advise treatment for verrucas if they are painful or spreading, for further information on this virus see the British Association of Dermatologists website.
Chilblains
Chilblains are a winter weather problem and are caused by an abnormal reaction of the skin to the cold. They are initially blue/purple and later become red and they either itch or burn, becoming increasingly painful, especially when the skin is warmed.
Chilblains are commonly found on extremities e.g. fingers, toes, noses and the tips of ears. On the feet they may be made worse by shoe pressure. They were very common in pre-war days before central heating was introduced.
However, they are still common in some people, particularly when the weather suddenly changes. The elderly, children and outdoor workers are especially at risk, but not everyone with cold feet will go on to develop chilblains.
Avoiding chilblains
Prevention of chilblains is much better than the cure! The secret is to change the temperature of the affected area slowly. Try these tips to minimise the problem:-
Do
Keep feet and legs warm – start wearing warm clothes before any cold spell.
Wear warm socks/tights – two thin layers are a good idea.
Wear thermal insoles and make sure your shoes are roomy enough to wriggle your toes.
Wear thick soled sensible shoes or boots to avoid pressure on the toes.
Wear bedsocks and use extra blankets if cold.
Try to go for a brisk walk daily and exercise your feet while sitting.
Have hot meals/drinks on cold days to help warm your whole body.
Consider taking dietary supplements to stimulate your circulation.
Don’t
Toast your feet by the fire or radiator.
Put a hot water bottle on cold feet.
Walk without slippers or socks.
Scratch the chilblains – you will only make them worse!
Treatment
If you do develop chilblains, they need treating according to the stage that they are at:
- For blue/purple looking chilblains, use suitable chilblain cream to stimulate the circulation. Your podiatrist or pharmacist will be able to advise you.
- For red, itchy, swollen chilblains, bathe feet in warm (not hot) water, dry carefully and use a soothing cream.
- For broken chilblains, bathe as above and apply a dry, sterile dressing to prevent infection.